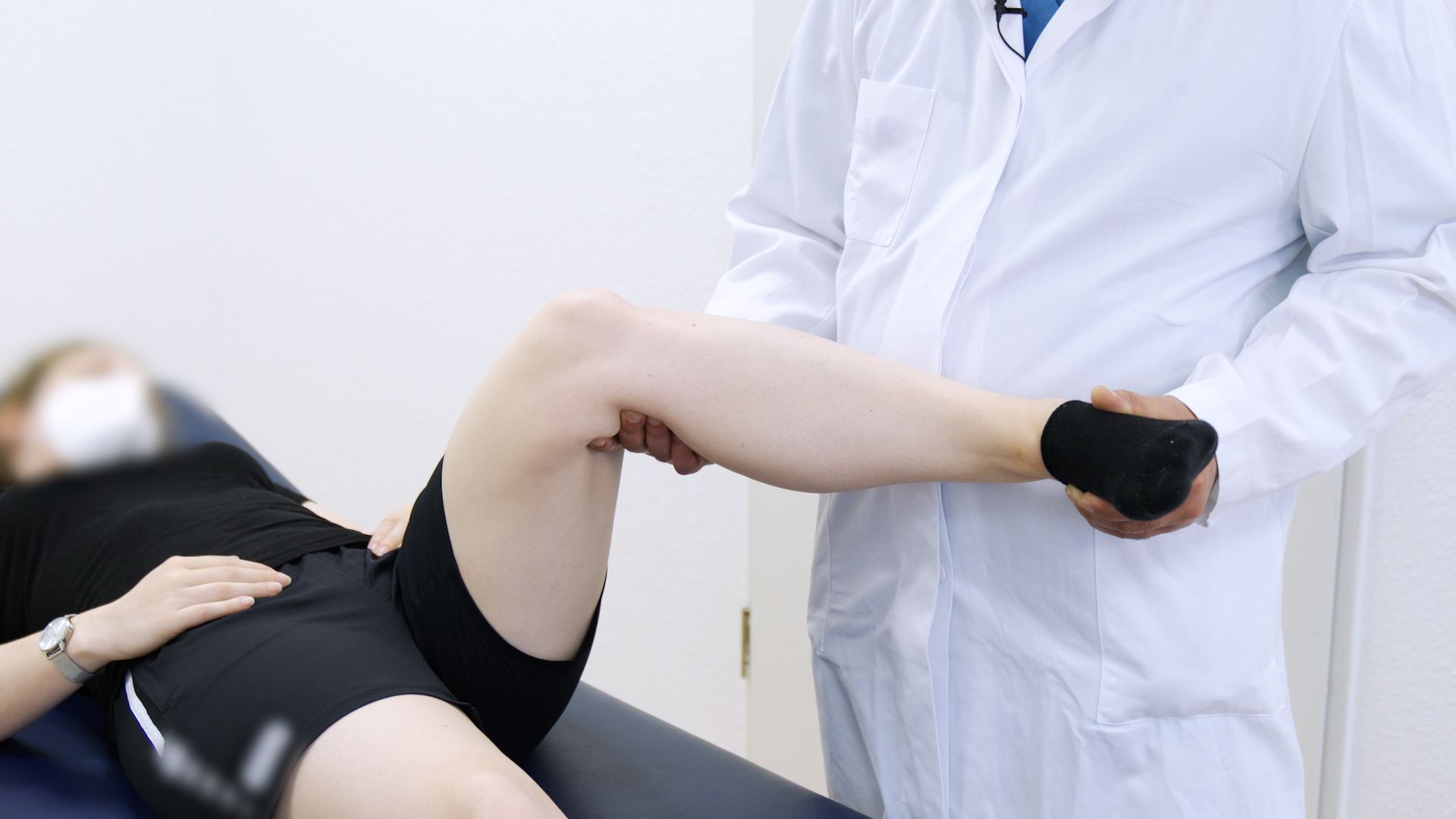
It is confusing and frustrating when you are told your scan is “fine,” but your knee still buckles. If you are dealing with knee instability normal MRI results, you are not alone, and it does not automatically mean “nothing is wrong.” A knee can give way because of ligament looseness that shows up best during movement, subtle or partial tears that are hard to see, meniscus injuries that are missed, or poor neuromuscular control after injury. This guide explains common knee giving way causes, why imaging can look reassuring while function is not, and which clinical tests and follow-up steps can help you and your clinician identify what is actually driving the instability.
1. When knee instability normal MRI happens, what it often means
In plain terms, “giving way” usually means your knee briefly loses control under load. Patients describe it as a sudden buckle, a shift, or a “slip” during cutting, pivoting, stairs, or stepping off a curb.
When someone has knee instability normal MRI findings, it often means one (or more) of these is true:
- The problem is functional and dynamic: the knee is unstable mainly during real-life motion, not when lying still in an MRI scanner.
- The injury is subtle: partial ligament injuries, small fiber disruptions, or healing injuries can be difficult to characterize on imaging.
- Another structure is contributing: meniscus, anterolateral structures, capsule, cartilage, or combined-injury patterns can drive symptoms even if the main ligament looks “intact.”
- Muscle timing and confidence are reduced: after injury, the brain may “guard” or react late, which can feel like instability even without a large tear.
If your report uses phrases like “sprain,” “mild laxity,” “equivocal,” or “no definite tear,” it can help to review an instability workflow with your clinician, because next steps are often guided by symptoms and exam, not imaging words alone.
2. Why an MRI can look normal even if something is wrong
MRI is excellent for many knee problems, but it is not a live stress test. MRI is a detailed snapshot of anatomy. Instability is a behavior of the joint, especially under speed, load, fatigue, and rotation. That mismatch is a major reason knee instability normal MRI scenarios occur.
2.1. Partial tears and “functionally insufficient” ligaments
A ligament can appear continuous yet still be functionally weak. This is one reason clinicians talk about partial ACL tear MRI sensitivity: the scan can miss fiber-level disruption or underestimate how much the ligament fails under force.
Newer imaging-focused reviews emphasize the complexity of diagnosing partial cruciate injuries and the need to integrate imaging with exam and history, including for partial PCL patterns (Dos Reis Morimoto et al. (2026)). This matters if you have recurrent shifting, but the report says “no full-thickness tear.”
Sometimes your symptoms align more with an occult ACL injury normal MRI situation: the ligament is not clearly torn on the images, but the knee behaves like it cannot control translation or rotation.
2.2. Meniscus lesions that are hard to see or easy to undercall
A meniscus can act like a stabilizer, especially in an ACL-injured knee. Certain tear locations can be subtle, and a meniscus tear missed on MRI can contribute to catching, pain with twisting, or the feeling that the knee “shifts” under load.
Ramp-type meniscus lesions (often at the back of the medial meniscus) have been highlighted as common in ACL reconstruction populations, with important imaging and arthroscopic correlations (Thaunat et al. (2021)). While that study focuses on surgical cases, the patient-level takeaway is practical: if your symptoms suggest a meniscus problem, a normal or “non-definitive” MRI does not always close the case.
2.3. Rotational stabilizers outside the ACL footprint
Some people have a pivoting, rotational “clunk” even if the ACL looks mostly intact. That can happen when injury involves the lateral capsule, iliotibial band-associated structures, or the anterolateral ligament injury spectrum.
There is growing attention to injuries around the lateral side, including the Kaplan fiber complex, which may be overlooked on initial assessment in “isolated” ACL injuries (Berthold et al. (2021)). Again, the practical point is not that MRI is “bad,” but that some stabilizing tissues are nuanced and can be missed or under-described.
If you want a clear explanation of why imaging and symptoms can diverge, this overview comparing MRI findings with functional instability assessment can help you frame questions for your next appointment.
3. Rotational instability: why the pivot shift can be positive with a normal MRI
Some patients do not mainly feel “front to back looseness.” Instead, they feel a twist and slide when the foot is planted and the body turns. That pattern is classic for rotational instability and is often discussed in the context of the pivot shift.
Patients searching for pivot shift test MRI normal are usually describing this: the knee may look acceptable at rest, but during a pivot, the tibia and femur briefly sublux and then reduce. This can feel like a sudden “jump” in the joint and is one of the more specific sensations people report after ACL-type injury.
In a post-surgical context, tibial-sided anterolateral ligament injuries have been associated with poorer healing and residual pivot shift on testing (Lee et al. (2025)). Even if you are not post-op, the message is relevant: rotational control depends on more than one structure, and a scan that focuses attention on the ACL alone may not fully explain a persistent pivoting symptom.
If your clinician documents a higher-grade pivot shift, it usually changes decision-making. This article on high-grade pivot shift findings explains why it is taken seriously and what it can mean for next steps.
4. How clinicians confirm (or rule out) true laxity when imaging is inconclusive
When knee instability normal MRI is reported, a careful exam becomes the anchor. The goal is to separate:
- Mechanical instability (true ligament laxity or meniscus-related subluxation)
- Functional instability (strength, motor control, proprioception, fear, or fatigue-related giving way)
- Pain inhibition (the knee “shuts off” due to pain, swelling, or irritation)
A helpful starting point is understanding what laxity means clinically, because “loose” on exam and “unstable” in real life overlap, but they are not identical.
4.1. The key hands-on tests (and what they actually tell you)
For ACL-type concerns, clinicians typically use a combination of maneuvers. If you want a patient-friendly overview, these tests are commonly discussed in clinic.
Core examples include:
- Lachman test: often the most sensitive bedside test for ACL laxity in many settings. If you want details on positioning and interpretation, see this Lachman test guide.
- Anterior drawer: can help, but may be limited by hamstring guarding.
- Pivot shift: most specific for rotational instability, but can be hard to elicit in a very tense or painful knee.
- Varus/valgus stress: screens for LCL/MCL injury patterns that can also cause giving way.
When patients ask about a clinical exam for ACL laxity, the important nuance is that a good clinician interprets tests together with your history (mechanism, swelling timing, “pop,” sports demands) and with side-to-side comparison.
If your MRI is normal but your story and exam do not match, it may be worth asking whether your assessment included a structured objective exam approach, because the “how” of testing can change accuracy.
4.2. A short decision aid for patients: what to do with conflicting results
If you have knee instability normal MRI results but recurrent episodes of giving way, this simple checklist can help you prepare for a follow-up visit:
- Describe the episode precisely: pivoting vs straight-line buckling, swelling after, ability to continue activity.
- Ask which instability pattern is suspected: translational (ACL), rotational (pivot shift), collateral, or combined.
- Confirm whether meniscus was suspected: especially if you have catching, locking, or pain with deep flexion and twist.
- Request side-to-side comparison findings: Lachman grade, pivot shift grade, endpoint quality.
- Discuss next-step testing: repeat exam after swelling settles, a second radiology read, additional sequences, or referral to a sports knee specialist.
4.3. When objective laxity measurement can add useful information
In some clinics, objective knee laxity testing is used to quantify side-to-side differences and help clarify borderline situations where symptoms are strong but imaging is equivocal; this can complement MRI by adding functional data rather than replacing it, as summarized in this overview of knee laxity testing approaches.
Depending on local availability, instrumented devices such as the GNRB arthrometer assessment or the Dyneelax knee arthrometer may be used to support clinical decision-making by quantifying laxity under standardized loads, while MRI remains important for evaluating associated meniscus, cartilage, and bone injuries.
If your symptoms feel “multi-directional” (for example, a mix of translation and rotation), clinicians may consider a more comprehensive approach like dynamic multi-axis laxity testing to better understand which plane of instability is driving the giving-way episodes.
5. What you can do next (and when to seek urgent care)
Persistent knee instability normal MRI symptoms deserve a plan, because repeated buckling can increase the risk of secondary injury (meniscus or cartilage) and can limit return to sport or even day-to-day confidence.
5.1. Practical next steps to discuss with your clinician
- Re-exam timing matters: swelling and pain can mask instability. A repeat exam 1 to 3 weeks later (or after rehab calms symptoms) can change findings.
- Rehab should be stability-driven, not just time-driven: ask whether your plan tracks objective stability, not only strength or range-of-motion milestones. This piece on rehab milestones vs stability metrics explains why people can “pass rehab” yet still feel unstable.
- Ask about combined injuries: especially if you have rotational symptoms, lateral pain, or repeated pivoting give-way events.
- Consider sport demands: cutting and pivoting athletes often need a higher stability threshold than someone who only walks or cycles.
For partial injuries, management can be individualized. In pediatrics, nonoperative pathways are sometimes used initially, with close monitoring and reassessment of stability and function (Hannon et al. (2026)). The same principle often applies to adults: if symptoms persist, the plan should evolve based on objective findings and real-world function.
5.2. Red flags: do not wait if you have these
Seek urgent assessment if you have any of the following:
- True locking (knee stuck and cannot fully straighten), which can suggest a displaced meniscus tear
- Rapid swelling after a new twist, fall, or pop
- Inability to bear weight or severe instability after an acute injury
- Fever, redness, or hot swollen joint (possible infection or inflammatory condition)
- New numbness or weakness in the foot or leg
6. Key takeaways and next steps
If you are stuck in the knee instability normal MRI loop, the most helpful mindset is that MRI is one input, not the whole answer. Giving way is often a sign of dynamic instability, and the “why” can include partial ligament injury, rotational stabilizer injury, meniscus lesions, or neuromuscular control problems.
Next steps that usually help:
- Bring a clear symptom description (what movement triggers it, swelling after, frequency).
- Ask for a focused instability exam and an explanation of your Lachman and pivot shift findings.
- Discuss whether additional assessment is needed when knee instability normal MRI does not match your function, including a second read, repeat exam, or objective measurement.
Diagnosis and treatment decisions should be clinician-led and individualized to your age, sport, and goals. The goal is not to “prove the MRI wrong,” but to identify what is causing the knee to behave unstably and then match the plan to that mechanism.
Clinical references (PubMed)
1) 2021 – Berthold et al. – High Rate of Initially Overlooked Kaplan Fiber Complex Injuries in Patients With Isolated Anterior Cruciate Ligament Injury. – Am J Sports Med – DOI: 10.1177/03635465211015682 – PMID: 34086492 – PubMed
2) 2021 – Thaunat et al. – Ramp Lesion Subtypes: Prevalence, Imaging, and Arthroscopic Findings in 2156 Anterior Cruciate Ligament Reconstructions. – Am J Sports Med – DOI: 10.1177/03635465211006103 – PMID: 33881943 – PubMed
3) 2026 – Dos Reis Morimoto et al. – Diagnosis and imaging assessment of partial anterior and posterior cruciate ligament tears. – Skeletal Radiol – DOI: 10.1007/s00256-026-05124-3 – PMID: 41555030 – PubMed
4) 2025 – Lee et al. – Tibial-sided Anterolateral Ligament Injuries Are Associated With Poor Healing and Residual Pivot Shift Testing After Anterior Cruciate Ligament Reconstruction. – Arthroscopy – DOI: 10.1016/j.arthro.2024.05.024 – PMID: 38849064 – PubMed
5) 2026 – Hannon et al. – Outcomes of Initial Nonoperative Management of Partial Anterior Cruciate Ligament Tears in Pediatric Patient. – J Pediatr Soc North Am – DOI: 10.1016/j.jposna.2026.100330 – PMID: 41908101 – PubMed