Rotational giving-way after ACL injury is not always explained by the ACL alone. The anterolateral complex knee is a functional set of lateral and capsular restraints that can influence how the tibia translates and internally rotates under load, shaping the pivot shift mechanism that clinicians feel at the bedside. Understanding this region matters when an “intact” graft still feels unstable, when MRI findings are borderline, or when a high-grade pivot shift suggests broader restraint failure. This guide summarizes current anatomy concepts, clinical exam implications, and what recent evidence says about lateral extra-articular tenodesis and anterolateral ligament procedures, with practical interpretation pitfalls for a clinician-led workup.
1. Anatomy and definitions: what clinicians mean by the anterolateral complex knee
In contemporary ACL practice, the anterolateral complex knee is less a single structure and more an ensemble of tissues that share a job: resisting coupled anterior translation and internal rotation, particularly in near-extension where pivoting episodes occur. Terminology varies across surgeons, radiologists, and biomechanical studies, so clarity about what is being discussed (and treated) is critical.
1.1 Key components and why “one ligament” is an oversimplification
Most descriptions of the anterolateral complex knee include combinations of:
- Anterolateral ligament related capsular thickening (variable appearance and definitions across studies and imaging protocols).
- Iliotibial band (ITB) and its deep connections (often discussed as important to anterolateral restraint in dynamic function).
- Anterolateral capsule and capsulo-osseous layers (important when capsular injury contributes to laxity).
- Adjacent lateral structures that influence coupled motion (lateral meniscus posterior root, lateral capsule, and bony morphology effects).
A practical clinic takeaway: “anterolateral” instability often reflects combined restraint behavior rather than an isolated tear you can point to on one slice of MRI.
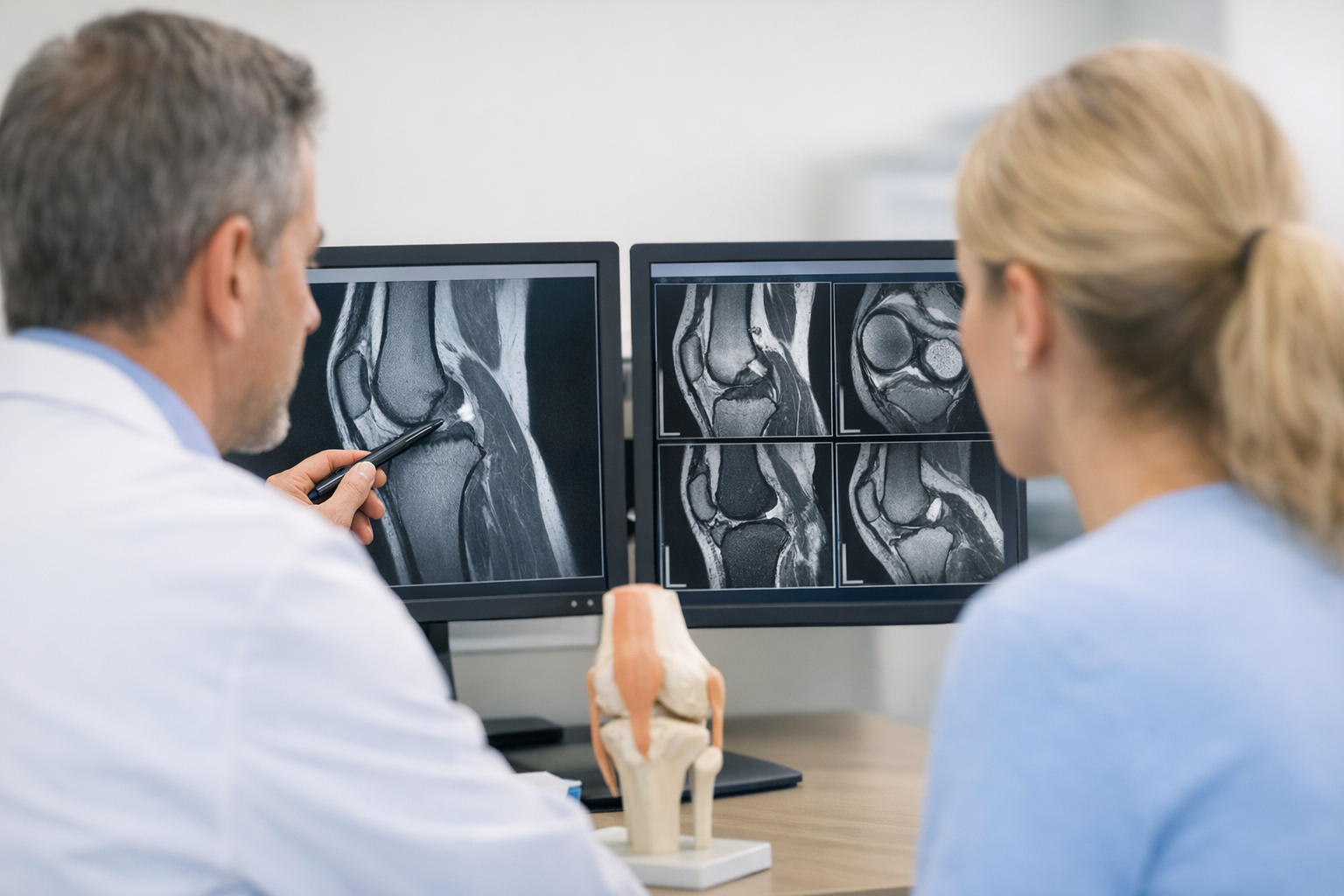
1.2 Imaging and terminology: what MRI can suggest and what it cannot prove
MRI can help identify capsular injury patterns, ITB abnormalities, Segond fracture, and associated meniscus or cartilage pathology. It also helps exclude alternative causes of lateral pain and instability. However, MRI is a static test and does not directly quantify the dynamic coupled motion that creates the pivot shift. Newer anatomic descriptions continue to refine how the lateral knee is conceptualized in imaging; for example, Saran et al. (2026) describes the lateral knee as a “W” configuration, reinforcing that multiple adjacent tissues can form a clinically relevant restraint ensemble rather than a single discrete band.
When documenting your assessment, it can help to explicitly separate:
- Structural findings (MRI, radiographs, prior op reports).
- Functional findings (pivot shift grade, side-to-side differences, symptoms during pivoting).
For contrast when considering “why lateral feels unstable,” reviewing medial plane stabilizers in ACL injury can help avoid attributing all rotational findings to the lateral side when valgus or medial restraint deficiency is also present.
2. Why the anterolateral complex knee matters for rotational knee instability and the pivot shift
The anterolateral complex knee is clinically relevant because the pivot shift is not purely “anterior tibial translation.” It is a coupled phenomenon involving internal rotation and a reduction event, typically felt as the lateral tibial plateau subluxes and then reduces with flexion. When anterolateral restraints are insufficient, the pivot shift may become easier to elicit, higher grade, and more symptomatic.
Two high-yield points for busy clinics:
- Rotational knee instability is often most obvious in sport-specific tasks (cutting, deceleration, change of direction) rather than in straight-line activities.
- A high-grade pivot shift can indicate a broader restraint problem than the ACL alone, especially in revision settings or patients with generalized laxity.
If you want a focused refresher on grading and clinical meaning, the discussion on high-grade pivot shift interpretation for anterolateral involvement provides a useful framework for tying exam findings to next-step decision making.
Mechanistically, the anterolateral complex knee interacts with the ACL to resist combined loads. In practice, that means some patients can have “acceptable” sagittal tests yet still report pivoting episodes, while others have obvious anterior laxity but minimal subjective rotation symptoms. Avoid over-generalizing from a single maneuver.
When considering augmentation procedures, remember that lateral extra-articular concepts are typically aimed at reducing pivot shift (rotational phenomena) rather than simply “tightening the knee” in a generic way.
3. Clinical assessment: exam maneuvers, interpretation pitfalls, and a decision aid
Evaluating suspected anterolateral contribution is about matching symptoms, exam, and context (primary ACL, revision, sport demands, laxity phenotype). The anterolateral complex knee is rarely “diagnosed” by a single test, but it can be inferred when the pattern of rotational laxity and symptoms persists or is disproportionate.
3.1 History features that should raise suspicion
- Giving-way episodes during pivoting even after rehab progress.
- Persistent lack of trust in the knee despite improving strength metrics.
- Instability described as “twisting out” more than “slipping forward.”
- Revision scenarios, particularly with a prior graft that looks intact on MRI but the patient reports rotational symptoms.
3.2 Exam maneuvers and common pitfalls
Core elements typically include:
- Lachman and anterior drawer (sagittal translation context).
- Pivot shift (primary clinical proxy for rotational behavior).
- Dial test and posterolateral corner screens when indicated (to avoid missing combined injury patterns).
- Varus-valgus stress testing (because coronal plane laxity can amplify perceived rotation).
Pitfalls to actively manage:
- Guarding and apprehension can reduce pivot shift sensitivity. Consider anesthesia exam data in operative planning when appropriate.
- Meniscus tears (especially lateral meniscus posterior horn/root pathology) can alter pivot behavior and should be assessed on MRI for surgical planning.
- Be cautious labeling “anterolateral failure” when PLC injury or generalized hyperlaxity is the primary driver.
For a broader framework that standardizes documentation and reduces missed elements, see this overview of the objective knee examination for instability assessment.
3.3 A short decision aid (clinician-led, no single-test dependency)
Use this as a quick synthesis tool rather than a rigid algorithm:
- Confirm the instability phenotype: is the complaint mainly pivoting (rotational) versus straight-line “slip” (sagittal) versus pain-driven pseudo-instability?
- Triangulate MRI and exam: MRI remains complementary and is typically needed to assess meniscus, cartilage, bone bruising, and for pre-op planning when reconstruction is considered.
- Escalate when discordant: in borderline or equivocal cases, consider adding objective instability quantification and revisit the working diagnosis and treatment plan.
For a practical example of connecting equivocal imaging to functional instability decisions, the borderline ACL MRI and instability testing workflow highlights where additional functional data may help clarify next steps without positioning any single tool as definitive.
4. Evidence summary: lateral extra-articular tenodesis, ALL reconstruction, and what recent studies support
When rotational laxity is clinically meaningful, surgeons may consider adding a lateral extra-articular procedure to ACL reconstruction. The intent is typically to reduce pivot shift and improve rotational control by supporting the anterolateral complex knee restraint function, particularly in higher-risk phenotypes.
4.1 Indications are risk-based, not purely anatomic
There is variation in how clinicians define “who needs augmentation,” but recent narrative and evidence summaries emphasize risk stratification rather than a one-size-fits-all approach. In Veizi et al. (2026), extra-articular tenodesis is discussed in terms of patient selection and technique considerations, reflecting the modern view that augmentation is most relevant when rotational instability risk is high (for example, high-grade pivot shift, revision ACLR, high-demand pivoting sport, or generalized laxity), while balancing potential downsides like over-constraint if performed inappropriately.
Systematic evidence syntheses also reinforce that “lateral procedures” include multiple techniques and heterogeneous cohorts. Migliorini et al. (2025) systematically reviewed ACL reconstruction using lateral extra-articular procedures, highlighting that interpretation must account for differences in surgical methods, outcomes, and follow-up windows.
4.2 Biomechanics: what cadaveric data can and cannot tell you
Cadaveric studies help isolate the mechanical effect of a procedure, but do not reproduce neuromuscular control, pain, or sport demands. Still, they can clarify whether a procedure meaningfully restores kinematics under controlled loads. In a matched-pair cadaveric model, Ihn et al. (2026) reports that lateral extra-articular tenodesis can restore rotational and translational stability regardless of fixation type, supporting the concept that extra-articular restraint can influence coupled laxity patterns relevant to pivot shift behavior.
Clinically, the question becomes: does the added control address the patient’s instability phenotype without creating unacceptable stiffness or altered kinematics? That remains a clinician-led decision integrating exam grade, sport demands, meniscal status, and prior surgery.
4.3 ALL reconstruction and clinical laxity outcomes
ALL reconstruction is one approach within the spectrum of anterolateral augmentation, and it is often discussed alongside, or compared with, tenodesis-style constructs. In a clinical comparison using laximetric outcomes, Vaz et al. (2025) compared a hamstring graft ACL reconstruction technique to the same approach combined with anterolateral ligament reconstruction, reflecting ongoing interest in how combined procedures influence function and measured laxity (without implying that any single technique is universally superior).
Because “measured stability” depends on how you measure it, technique comparison is strengthened when studies report both patient outcomes and standardized laxity quantification. For a technique-focused discussion of construct variations, this study comparing 1-strand vs 2-strand ACL plus ALL reconstruction illustrates how procedural details may influence stability endpoints and how careful interpretation is required across cohorts.
4.4 Procedure effects beyond rotation: avoid assuming every change is beneficial
Extra-articular procedures are principally designed to address rotation, but they may also influence sagittal translation depending on tensioning, fixation, and knee position at fixation. When interpreting outcomes, separate “pivot shift improvement” from “overall stiffness” and monitor extension, flexion, and functional progression. A relevant example is the Dyneelax-based analysis discussed in whether lateral extra-articular tenodesis affects sagittal knee laxity, which frames how adding a lateral procedure may be evaluated with objective laxity metrics rather than assumption alone.
Ultimately, the goal is not to “tighten everything,” but to restore stable, confident motion that matches the patient’s demands while protecting the graft and associated structures. In that context, the anterolateral complex knee is a functional target: it matters most when its deficiency is clinically expressed as symptomatic pivoting.
5. Quantifying rotational control: where instrumented data can complement exam and MRI
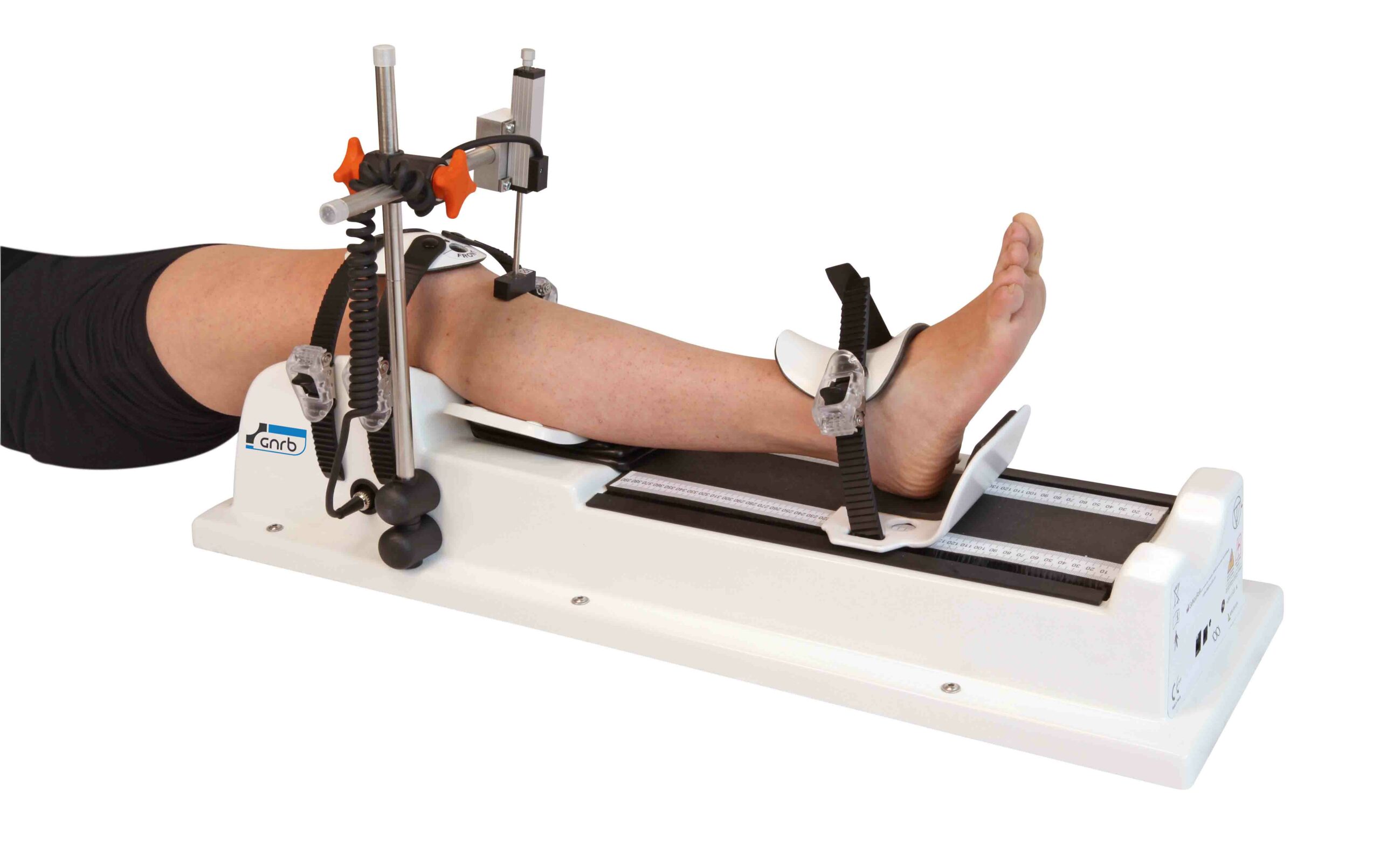
Even in experienced hands, the pivot shift is partly subjective and can vary with relaxation, examiner technique, and patient morphology. When you suspect an anterolateral contribution, instrumented knee laxity testing can add repeatable side-to-side quantification that complements clinical examination and MRI by capturing functional instability patterns that imaging alone may not fully reflect.
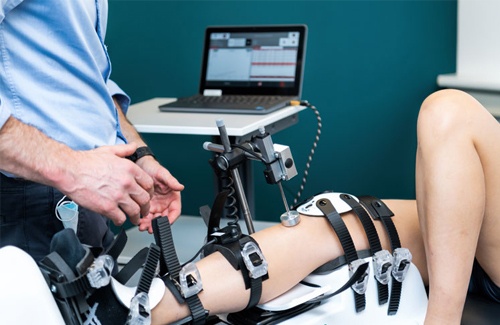
In clinics that use a multi-axis approach, an automated arthrometer can help standardize load application and document change over time, which is particularly relevant when the anterolateral complex knee is suspected to contribute to persistent rotation symptoms despite apparently acceptable sagittal laxity.
- For sagittal ACL laxity quantification, an example is the GNRB arthrometer for ACL assessment.
- For workflows that incorporate multiple planes and dynamic response, the Dyneelax knee arthrometer is designed to support standardized, repeatable measurements.
Two practical integration points (without overclaiming):
- If you are building a standardized protocol, this multi-axis dynamic knee laxity testing workflow shows how objective data can be organized alongside exam and imaging.
- When interpreting measurement quality and repeatability in injured cohorts, the Dyneelax reliability study in knee ligament injury evaluation is an example of how reliability is assessed and reported.
Objective laxity metrics are also increasingly studied in relation to tissue-level signals on imaging. For example, this report on the relationship between quantitative MRI UTE-T2 and measured knee laxity after ACL reconstruction illustrates how imaging biomarkers and functional stability measures may be paired in research and follow-up, reinforcing that these modalities are best viewed as complementary rather than interchangeable.
6. Key takeaways and next steps
- The anterolateral complex knee is best understood as a restraint ensemble that can meaningfully influence pivot shift behavior and symptomatic rotational instability.
- MRI remains complementary and is important for associated injury assessment, but it does not directly quantify dynamic pivoting or side-to-side functional laxity.
- High-grade pivot shift, revision context, laxity phenotype, and sport demands often drive consideration of lateral augmentation more than a single “ALL tear” finding.
- When adding procedures such as lateral extra-articular tenodesis or anterolateral ligament procedures, interpret outcomes through both patient function and measured stability, while avoiding over-constraint.
For performance-phase decision making, especially when you need to align clinical exam, functional testing, and stability metrics, review return-to-sport criteria incorporating objective knee stability metrics. A structured follow-up plan can help determine whether persistent pivoting reflects residual rotational laxity, neuromuscular control deficits, meniscal pathology, or a combination that warrants re-evaluation.
7. Clinical references (PubMed)
1) 2026 – Veizi et al. – Extra-articular Tenodesis for ACL Reconstruction: Who Needs it and is there a Superior Technique? – Curr Rev Musculoskelet Med – DOI: 10.1007/s12178-026-10028-9 – PMID: 41922887 – PubMed
2) 2026 – Saran et al. – Crucial anatomic ensemble of the lateral knee: the ‘W’ configuration. – Clin Radiol – DOI: 10.1016/j.crad.2026.107288 – PMID: 41814107 – PubMed
3) 2025 – Migliorini et al. – Anterior Cruciate Ligament Reconstruction Using Lateral Extra-Articular Procedures: A Systematic Review. – Medicina (Kaunas) – DOI: 10.3390/medicina61020294 – PMID: 40005410 – PubMed
4) 2026 – Ihn et al. – Lateral Extra-articular Tenodesis Restores Knee Rotational and Translational Stability Regardless of Fixation Type: A Matched-Pair Cadaveric Study. – Am J Sports Med – DOI: 10.1177/03635465261428673 – PMID: 41877535 – PubMed
5) 2025 – Vaz et al. – Anterior cruciate ligament reconstruction using hamstring graft: Functional and laximetric results of a pedicled semi tendinosus technique compared to a pedicled semi tendinosus technique combined with anterolateral ligament reconstruction. – Orthop Traumatol Surg Res – DOI: 10.1016/j.otsr.2025.104311 – PMID: 40466755 – PubMed