Acute knee trauma is common in urgent and emergency settings, but soft tissue injuries are frequently missed when pain, swelling, or limited exam conditions obscure key signs. This workflow is an acute knee injury algorithm designed for rapid risk stratification, safe early management, and consistent documentation, with special attention to suspected ACL and multi-ligament patterns. The aim of knee ligament injury triage is not to “name the exact tear” at first contact, but to (1) rule out time-critical threats, (2) identify patients who need early specialist input, and (3) ensure appropriate imaging and follow-up so instability is not diagnosed weeks later. Service audits and pathway reviews highlight that delays in diagnosis and onward referral can be common without a structured approach.
Knee ligament injury triage step 1: Immediate threats and “do not miss” patterns
Start by separating limb-threatening and time-sensitive injuries from isolated sprains. This first step of knee ligament injury triage should happen before a detailed laxity exam.
Red flags that change your pathway now
- Neurovascular risk: absent or asymmetric pulses, cool foot, delayed cap refill, new paresthesia, foot drop.
- Gross instability or deformity: suspicion of knee dislocation multiligament injury (including spontaneously reduced dislocation).
- Locked knee (true mechanical block to extension), large effusion, or inability to bear weight after a twisting injury (consider displaced meniscal tear and urgent ortho pathway). See Rhind et al. (2024) for clinical framing of the locked knee presentation.
- Extensor mechanism failure: inability to straight-leg raise, high-riding patella, palpable gap.
- Open injury, suspected septic arthritis (fever, hot swollen joint, systemic features), or compartment syndrome features.
Immediate actions: analgesia, immobilize if grossly unstable, document neurovascular status (including peroneal nerve function), and escalate for urgent orthopedic and vascular assessment when indicated. For structured bedside sequencing once stabilized, consider the exam order described in objective knee examination in orthopaedics.
Step 2: Fracture exclusion and first-line imaging (do this before stressing the knee)
If fracture is plausible, prioritize radiographs before provocative testing. Use the Ottawa knee rules to guide when plain films are indicated, and document the criteria you applied. In knee ligament injury triage, this reduces missed fractures and helps justify imaging decisions.
When CT is considered
CT may be used for complex fracture patterns or when X-ray findings are unclear. Emerging imaging approaches are being explored, including photon-counting CT for integrated assessment of acute knee injury, but this is not yet standard in most urgent care pathways (see Zijta et al. (2025)).
Effusion clues: identify hemarthrosis early
A tense effusion within hours after a non-contact pivot or contact twist can suggest traumatic knee effusion hemarthrosis, which should raise suspicion for ACL rupture, osteochondral injury, or significant intra-articular damage. Early aspiration is clinician-dependent and context-specific, but careful documentation of onset, volume, and tension helps downstream diagnostic accuracy and can improve the quality of urgent care ACL injury diagnosis.
Step 3: Focused history that actually drives decisions
The history should narrow your differential and determine how aggressive your knee ligament injury triage needs to be. A useful approach is to record a short “mechanism plus immediate sequelae” bundle:
- Mechanism: valgus collapse, hyperextension, dashboard-type posterior force, direct varus blow, twisting with planted foot.
- Sound/sensation: “pop” at injury, feeling of shift or giving way.
- Function: immediate inability to continue sport, later episodes of instability.
- Swelling timing: within 2 to 6 hours vs next day.
- Prior instability or surgery: prior ACL reconstruction, contralateral injury.
If you need a quick symptom cross-check that aligns with patient language, the cues outlined in did I tear my ACL can help structure your questions without over-promising a diagnosis in the urgent setting.
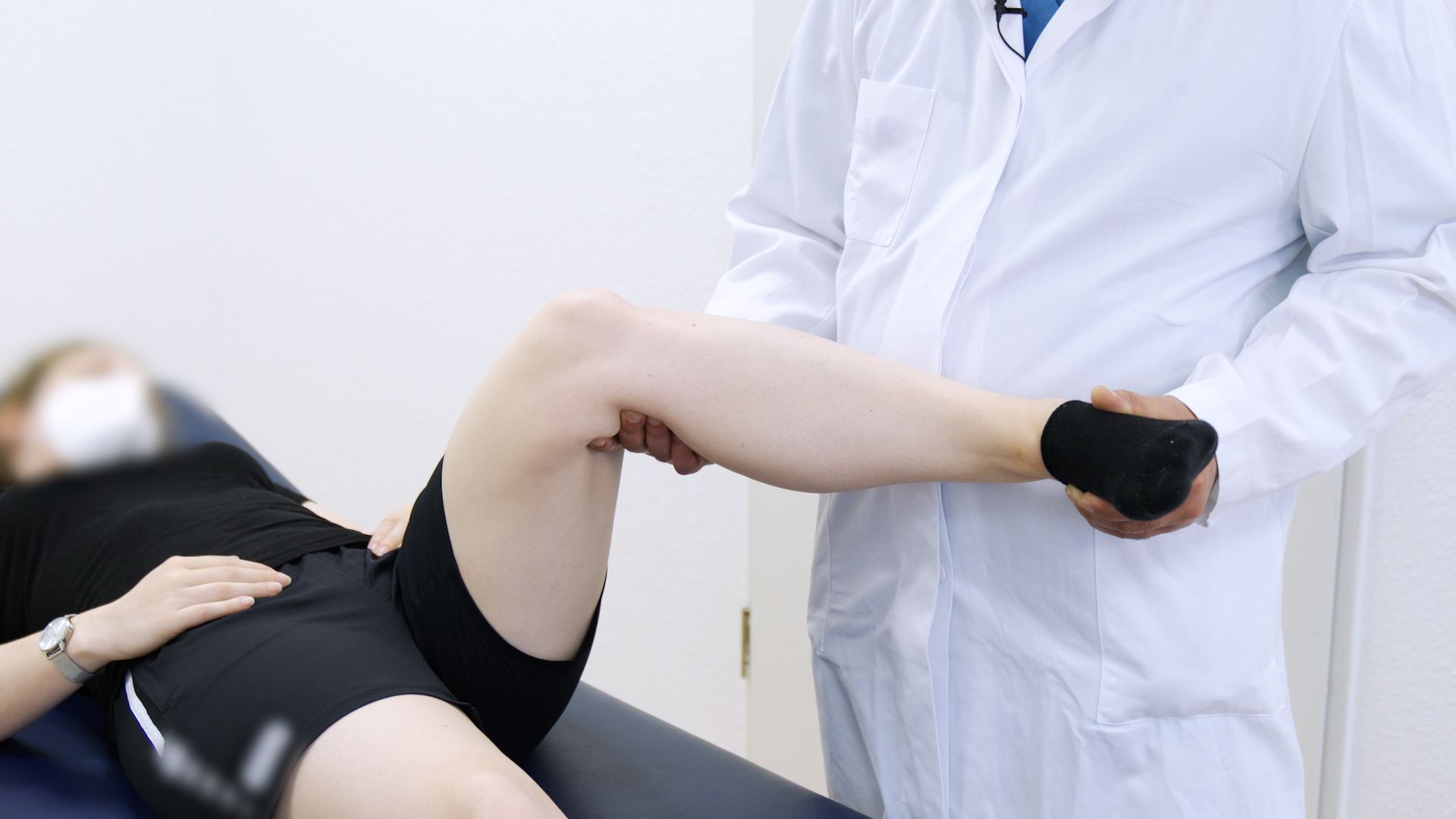
Step 4: Bedside exam workflow for suspected ligament injury (when, why, pitfalls)
In urgent care, pain, guarding, and swelling reduce the reliability of manual tests. Still, a consistent sequence improves comparability and reduces missed multi-structure injuries. This is the “engine room” of knee ligament injury triage.
Exam sequence (repeatable and documentable)
- Inspect: effusion, bruising, alignment, quadriceps inhibition, patella position.
- Palpate: joint lines, MCL/LCL, fibular head, posterolateral corner tenderness, tibial plateau.
- ROM: active and passive, end-feel, painful blocks.
- Neurovascular: pulses, cap refill, peroneal nerve motor and sensation.
- Targeted ligament tests: choose based on mechanism and tolerance.
For a concise list of core bedside maneuvers and how they complement each other, see top 6 ACL diagnostic tests.
ACL: Lachman first, then pivot when appropriate
Lachman is often the most practical early ACL test. Record both the amount of translation and the endpoint quality, and compare to the contralateral side. When documenting, be explicit about pain/guarding and whether swelling limited the exam, because these factors affect Lachman test accuracy. For technique and interpretation points that matter in triage notes, follow the Lachman test guide for ACL injury detection.
The pivot shift test is highly informative for rotational instability but is frequently limited in acute settings by guarding and pain. Consider deferring pivot shift until analgesia improves, swelling decreases, or specialist review, and document why it was not performed. When you suspect ACL injury but the bedside picture is mixed, review common diagnostic traps in ACL tear detection.
Collateral ligaments and posterolateral corner: do not stop at “ACL only”
- Valgus stress at 0 and 30 degrees: suggests MCL and, at 0 degrees, possible multi-ligament involvement.
- Varus stress at 0 and 30 degrees: suggests LCL, and at 0 degrees consider cruciates and capsule.
- Posterior drawer and posterior sag: consider PCL injury, especially with dashboard mechanism.
- Dial test and posterolateral symptoms: consider PLC injury, especially with varus hyperextension.
If you need language that correctly conveys instability rather than just pain, it helps to align documentation with the concept explained in what knee laxity means and why it matters.
Conditional tech integration: when objective laxity testing can support urgent decisions
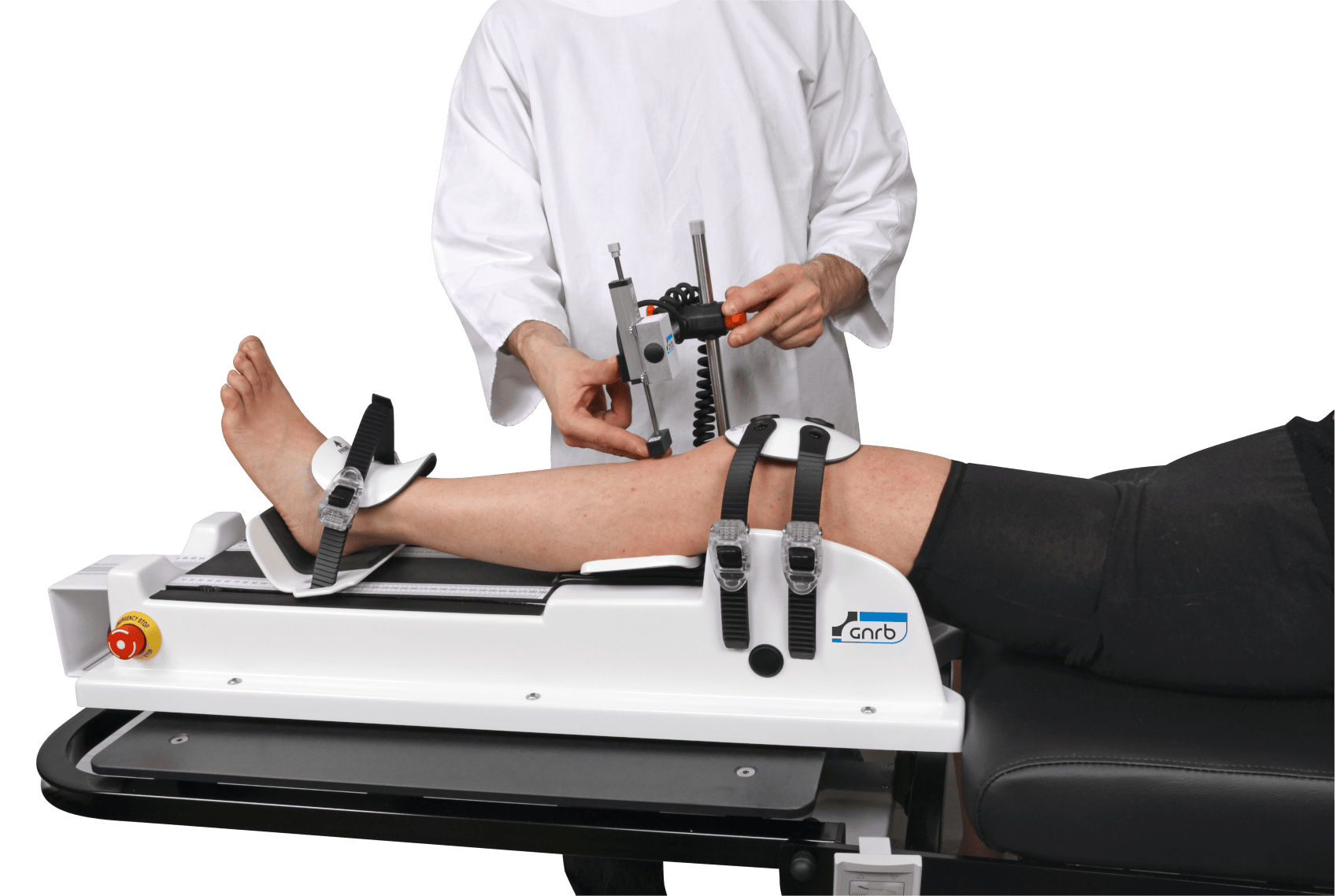
When manual findings are equivocal due to pain, guarding, or borderline end-feel, knee laxity testing with instrumented methods may help quantify side-to-side differences and support consistent follow-up decisions, while remaining complementary to clinical exam and MRI. An overview of options is summarized in knee laxity testing, and dynamic considerations are discussed in dynamic knee testing.
In pathways that have access, instrumented assessment such as the GNRB arthrometer for ACL assessment or the Dyneelax knee arthrometer can be used as diagnostic support to quantify functional instability (for example in suspected partial ACL tears or uncertain exams). It should not be positioned as a replacement for MRI, because MRI remains important for associated meniscal, cartilage, and bony injury assessment and for surgical planning when reconstruction is considered. For a balanced discussion of how these tools may complement imaging in selected workflows, see MRI vs arthrometer for improving ACL tear detection.
knee ligament injury triage step 5: Disposition, documentation, and referral timing
Disposition decisions are where knee ligament injury triage either prevents delays or creates them. Reviews of acute ACL pathways emphasize that variability in early assessment and follow-up contributes to delayed diagnosis and downstream inefficiency (see Allott et al. (2022)). Service redesign work also highlights avoidable time loss between first contact, imaging, and specialist review (see Vindya et al. (2025)), and system disruption can further amplify delays (see Pattnaik et al. (2023)).
Decision aid: three practical triage buckets
-
Urgent same-day or next-day orthopedics
- Suspected knee dislocation or multi-ligament injury pattern, neurovascular concerns, or gross instability.
- True locked knee or suspected displaced meniscal tear with mechanical block.
- Extensor mechanism disruption.
-
Early specialist or sports medicine referral (often within 1 to 2 weeks)
- High suspicion ACL tear with giving way, large hemarthrosis, or clear positive Lachman despite acute pain.
- Suspected combined injuries (ACL plus MCL, PLC, or PCL features).
- Recurrent instability episode after initial injury.
In documentation and discharge instructions, explicitly answer: when to refer to orthopedics knee injury and what triggers immediate return (new neurovascular symptoms, escalating pain, progressive swelling, inability to weight bear).
-
Conservative pathway with safety-netting
- Mild pain-limited laxity exam without clear instability, no red flags, and improving function.
- Plan: early re-exam once swelling and guarding settle, plus physiotherapy input where appropriate.
Minimum documentation set (high yield for continuity)
- Mechanism, swelling timing, ability to continue activity.
- Neurovascular exam (including peroneal nerve).
- Effusion presence (and whether tense), ROM limits, weight-bearing status.
- Which tests were done (Lachman, drawer, varus/valgus, pivot shift) and why others were deferred.
- Working impression phrased cautiously (for example “suspected ACL injury” rather than definitive labeling).
When your triage impression is ACL-focused, it can help to align terminology with a standard overview such as ACL injury (anterior cruciate ligament tear), particularly for shared decision-making and consistent follow-up planning in urgent care ACL injury diagnosis.
Closing: Key takeaways and next steps
Effective knee ligament injury triage is mainly about sequencing: stabilize and rule out threats first, image appropriately, then perform a structured ligament exam that you can reproduce and document. When swelling and pain limit accuracy, treat the first visit as the start of a pathway, not the end of a diagnosis. Re-examination after guarding settles, early referral for high-risk patterns, and clear safety-net instructions reduce missed instability and delayed care.
Next steps: apply this workflow, document the minimum dataset, and ensure every patient leaves with a specific plan for reassessment or referral. If your service is improving pathways, consider auditing time-to-diagnosis and time-to-specialist review as quality markers within knee ligament injury triage.
Clinical references (PubMed)
1) 2022 – Allott et al. – Evaluating the diagnostic pathway for acute ACL injuries in trauma centres: a systematic review. – BMC Musculoskelet Disord – DOI: 10.1186/s12891-022-05595-0 – PMID: 35799147 – PubMed
2) 2025 – Vindya et al. – A Retrospective Audit of the Timescales Involved in the Diagnosis and Management of Soft Tissue Knee Injuries at a Single National Health Service Trust: A Quality Service Improvement and Redesign Project. – Cureus – DOI: 10.7759/cureus.94641 – PMID: 41104036 – PubMed
3) 2023 – Pattnaik et al. – Navigating ACL Injuries Amid the COVID-19 Pandemic: A Retrospective Analysis. – Cureus – DOI: 10.7759/cureus.47857 – PMID: 38022222 – PubMed
4) 2025 – Zijta et al. – The emerging role of photon-counting detector CT: primary experience on the integrated assessment of acute knee injuries. – Eur Radiol Exp – DOI: 10.1186/s41747-025-00616-8 – PMID: 40783626 – PubMed
5) 2024 – Rhind et al. – The locked knee. – Br J Hosp Med (Lond) – DOI: 10.12968/hmed.2022.0215 – PMID: 38300674 – PubMed