Distinguishing ACL graft stretch vs failure is a common, high-stakes clinical decision after reconstruction because symptoms can look similar while management differs. Athletes may describe giving way, distrust, or a “new normal” instability that can also be driven by pain, swelling, neuromuscular inhibition, or associated meniscal injury. The challenge is to decide whether you are seeing graft elongation after ACL reconstruction, a true graft rupture, or a non-graft cause of recurrent symptoms. This workflow is designed for sports physicians and physiotherapists to structure history, examination, imaging, and objective testing so that decisions remain evidence-based, cautious, and clinician-led.
1. Defining ACL graft stretch vs failure in practice
In day-to-day clinics, ACL graft stretch vs failure is rarely a binary diagnosis made from a single data point. It is a synthesis of:
- Symptoms (giving way, apprehension, inability to trust pivoting)
- Function (return-to-sport trajectory vs plateau/regression)
- Examination (translation, endpoint quality, pivot shift, rotational control)
- Context (time from surgery, new trauma, rehab quality, swelling)
- Structural assessment (MRI and radiographs when indicated)
Working definitions (clinical, not absolute)
- “Stretch” / elongation phenotype: gradually increasing anterior translation and/or pivot symptoms with a graft that may still be continuous on MRI, often with a softer endpoint and functional instability under dynamic tasks.
- “Failure” phenotype: clear traumatic event or progressive instability with imaging and/or exam suggesting rupture, major attenuation, fixation failure, tunnel issues, or associated constraints (meniscus, PLC) no longer compensating.
Keep expectations time-specific. Early rehabilitation can include transient swelling-related inhibition and variable perceived stability, while persistent or progressive residual anterior laxity after ACLR beyond expected milestones should prompt structured reassessment. A helpful clinical baseline is to revisit the intended recovery trajectory and red flags described in ACL reconstruction surgery diagnosis and recovery timelines.
When framing ACL graft stretch vs failure, explicitly document: “Is this a stability complaint, a confidence complaint, or both?” The downstream workup is different.
2. Early signs and pitfalls that mimic graft problems
Clinically, early ACL graft failure signs can be obvious (new pivoting injury with swelling and instability) or subtle (a slow drift in stability metrics during advanced training). Many patients first report recurrent instability after ACL surgery only when they reintroduce rotation, deceleration, or contact drills.
2.1. Patient-reported clues that should trigger reassessment
- New “giving way” episodes during pivoting or cutting (especially if reproducible)
- New effusion pattern after instability events (think meniscal or chondral involvement)
- Apprehension that is task-specific (pivot tasks) rather than global fear
- Plateau or regression in hop testing, deceleration, or sport-specific drills
For relapse mechanisms, common warning patterns, and how symptoms evolve over time, align your questioning with warning signs after ACL surgery.
2.2. Common “false positives” for ACL graft stretch vs failure
Before concluding ACL graft stretch vs failure, actively exclude contributors that can inflate perceived instability:
- Arthrogenic muscle inhibition (AMI) with quadriceps shutdown, altered landing mechanics, and protective movement patterns
- Pain-driven guarding that changes endpoint feel or pivot tolerance
- Meniscal pathology (especially ramp lesions, root tears) that can increase dynamic translation
- Posterolateral corner (PLC) or MCL laxity that amplifies rotational symptoms
AMI and fear can meaningfully distort performance and even perceived laxity; consider the pathway discussed in AMI-related laxity and kinesiophobia after ACL reconstruction before labeling structural failure.
2.3. A short decision aid for first-pass triage
- High concern: new trauma + swelling + new instability episodes, or a clearly positive pivot shift that is new compared with prior notes.
- Intermediate concern: progressive instability without clear trauma, especially with measurable side-to-side change over serial exams.
- Lower concern: primary complaint is pain, stiffness, or fear with stable objective findings and no giving-way history.
This triage does not “diagnose” ACL graft stretch vs failure, but it determines urgency and the breadth of differential.
3. Workflow to investigate suspected elongation or rupture
This section operationalizes the differential diagnosis graft stretch vs rupture. It is designed to standardize how you evaluate ACL graft stretch vs failure when an athlete presents with instability, plateaued progress, or re-injury concern.
3.1. Step 1: Reconstruct the timeline and load exposure
- Time from surgery, graft type, fixation method (if known), prior laxity notes
- Return-to-running, return-to-cutting, and contact exposure dates
- Any sentinel event (pivot, contact, awkward landing) and immediate effusion
- Recent training spikes, fatigue, or change in surface/footwear
When revision is on the table, categorize failure mechanisms and contributing factors. A practical framework is summarized in causes and evaluation pathways for failed ACL reconstructions, and a broad etiology and revision overview is discussed in Capece et al. (2026).
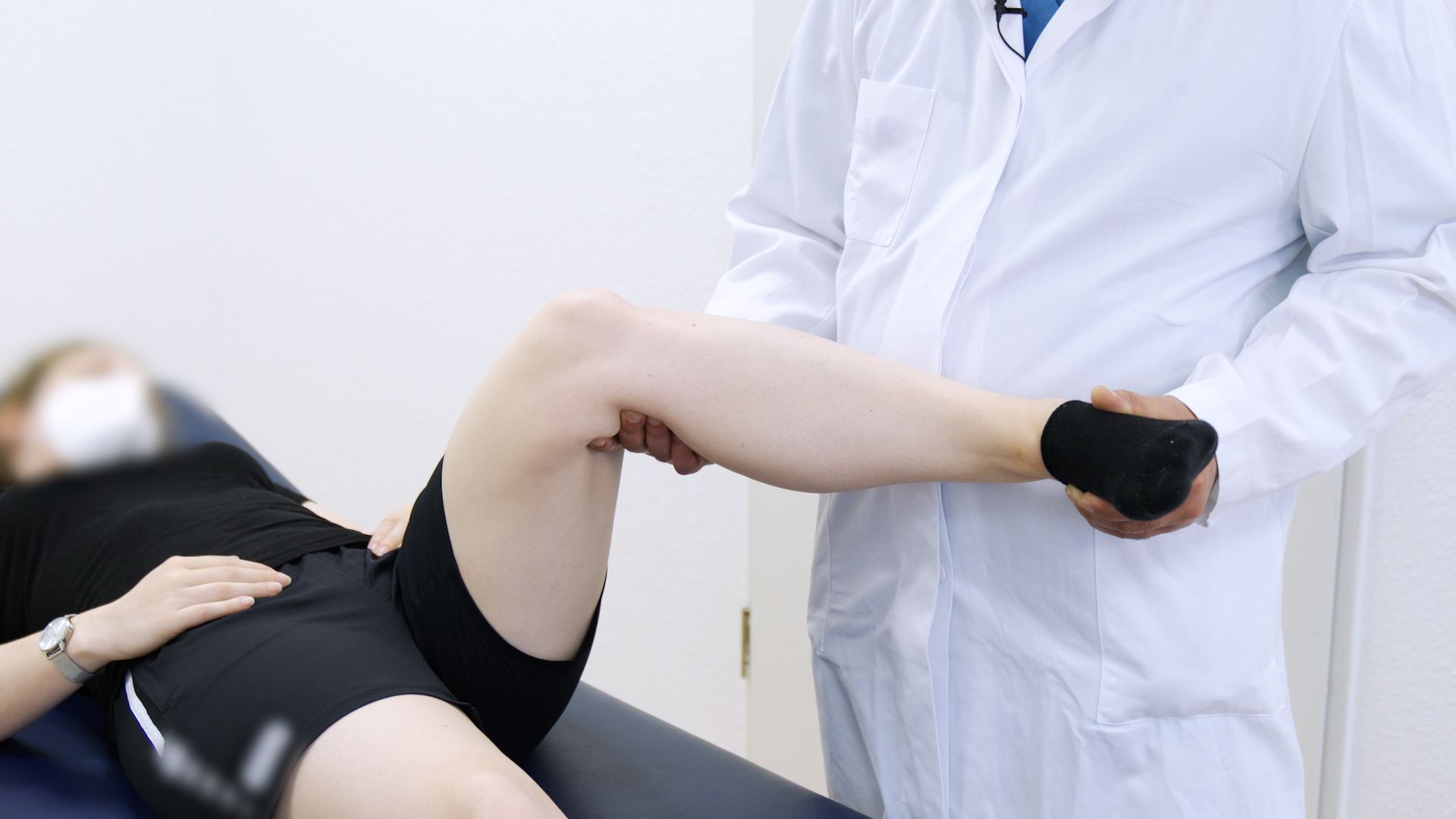
3.2. Step 2: Focused exam for translation, endpoint, and rotation
At minimum, document swelling, ROM, joint line tenderness, and then perform clinical tests for ACL graft integrity in a consistent order:
- Lachman: translation and endpoint quality, compared side-to-side
- Anterior drawer: less sensitive early, but useful adjunct
- Pivot shift: rotational instability and functional subluxation behavior
- Varus/valgus stress: screen MCL/LCL contributions
- Dial test (when indicated): rotational laxity, PLC suspicion
If your Lachman documentation varies between clinicians, standardize technique using the Lachman test guide. Also consider anchoring your clinic notes to a reproducible exam template such as objective knee examination in orthopaedics.
Pitfall: a “guarded” patient can appear to have a firmer endpoint, while a painful knee can be harder to pivot, both masking ACL graft stretch vs failure. If pain limits exam quality, treat the irritability first and re-test, or move earlier to objective measurement and imaging.
3.3. Step 3: Quantify side-to-side change and trend it
One-off findings can mislead. When you suspect ACL graft stretch vs failure, try to compare with prior documented values and add objective measures when possible. A broad map of options is in the knee laxity testing overview.
Clinically relevant questions:
- Is laxity stable, improving, or worsening over serial visits?
- Does laxity increase under higher load or after fatigue?
- Is rotational instability (pivot shift) disproportionate to anterior translation?
This is where “symptoms vs structure” separation becomes clearer: a patient with high fear but stable side-to-side measures may need a different plan than a patient whose measures drift over weeks.
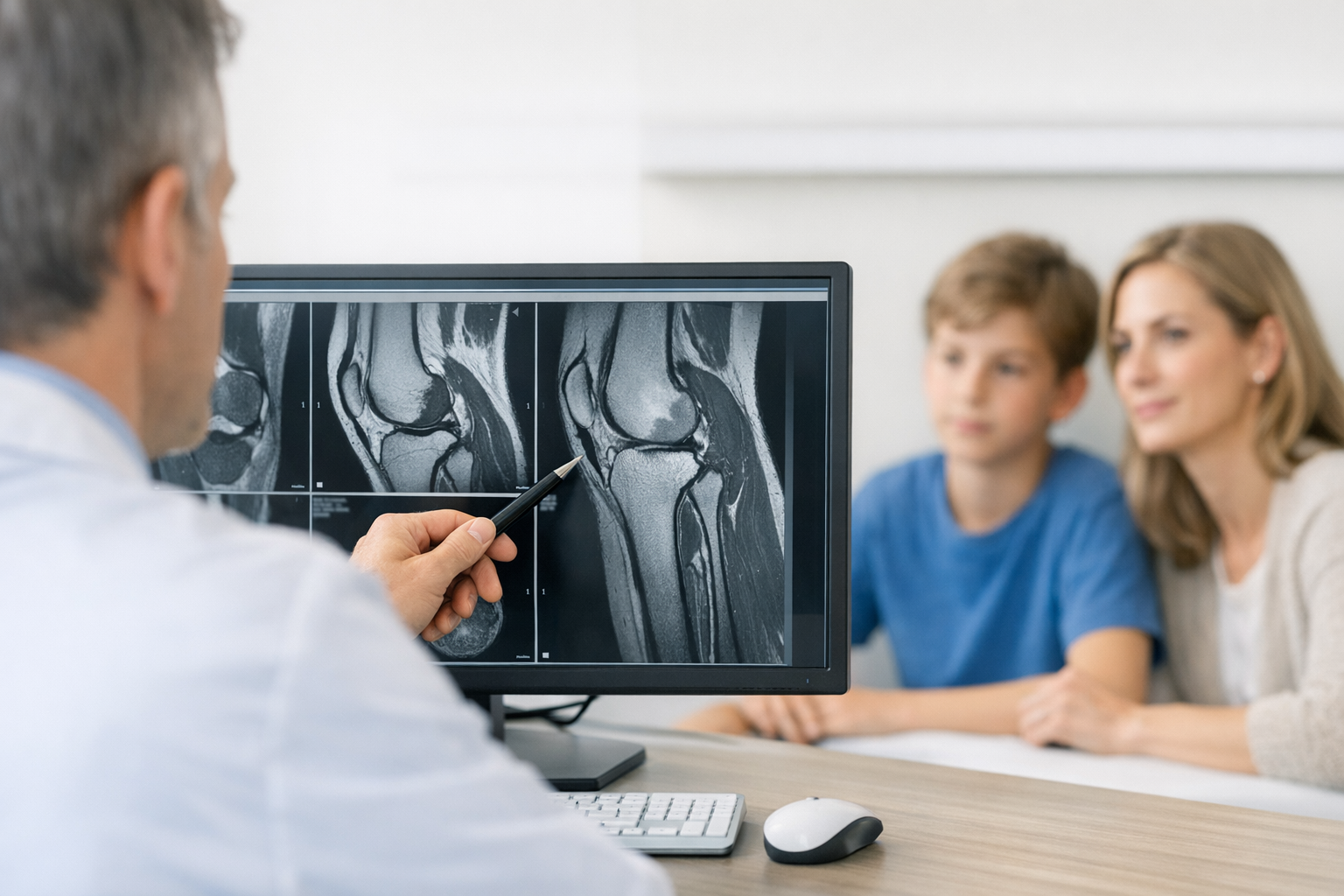
3.4. Step 4: Imaging strategy that answers the right question
MRI is typically used to evaluate graft continuity, tunnel position, cyclops lesions, menisci, cartilage, and bone bruising patterns. In suspected ACL graft stretch vs failure, the most useful MRI question is not only “Is it torn?” but “What else is driving instability or symptoms?”
Document MRI findings of ACL graft failure cautiously because imaging can be equivocal in partially disrupted, attenuated, or remodeled grafts. In practice, MRI interpretation is strongest when integrated with objective instability metrics and a clear mechanism history. A balanced discussion of strengths and limitations is covered in MRI vs arthrometer in suspected ACL tear detection.
When you have access to advanced graft imaging sequences or quantitative approaches, consider how imaging biomarkers relate to measured laxity. An example of this integration is discussed in quantitative MRI UTE-T2 and postoperative laxity.
3.5. Step 5: Decide on management direction and urgency
Management is guided by function, objective instability, and associated injury burden, not by one test. If objective instability and symptoms align, consider whether you are dealing with isolated laxity, rotational deficiency, technical factors (tunnel placement, graft bending angles), or new trauma.
Radiographic parameters can matter in revision planning. For example, graft bending angle considerations in failed reconstructions are explored in Weiss et al. (2026). Sport demands and graft selection considerations can also influence the evaluation pathway, as highlighted in Abu Mukh et al. (2026).
Use clear language in notes: “Findings suggest instability consistent with ACL graft stretch vs failure, with X objective laxity pattern and Y rotational finding; MRI requested to assess graft integrity and associated injuries; plan depends on combined findings.”
4. Objective laxity and rotational assessment in suspected graft compromise
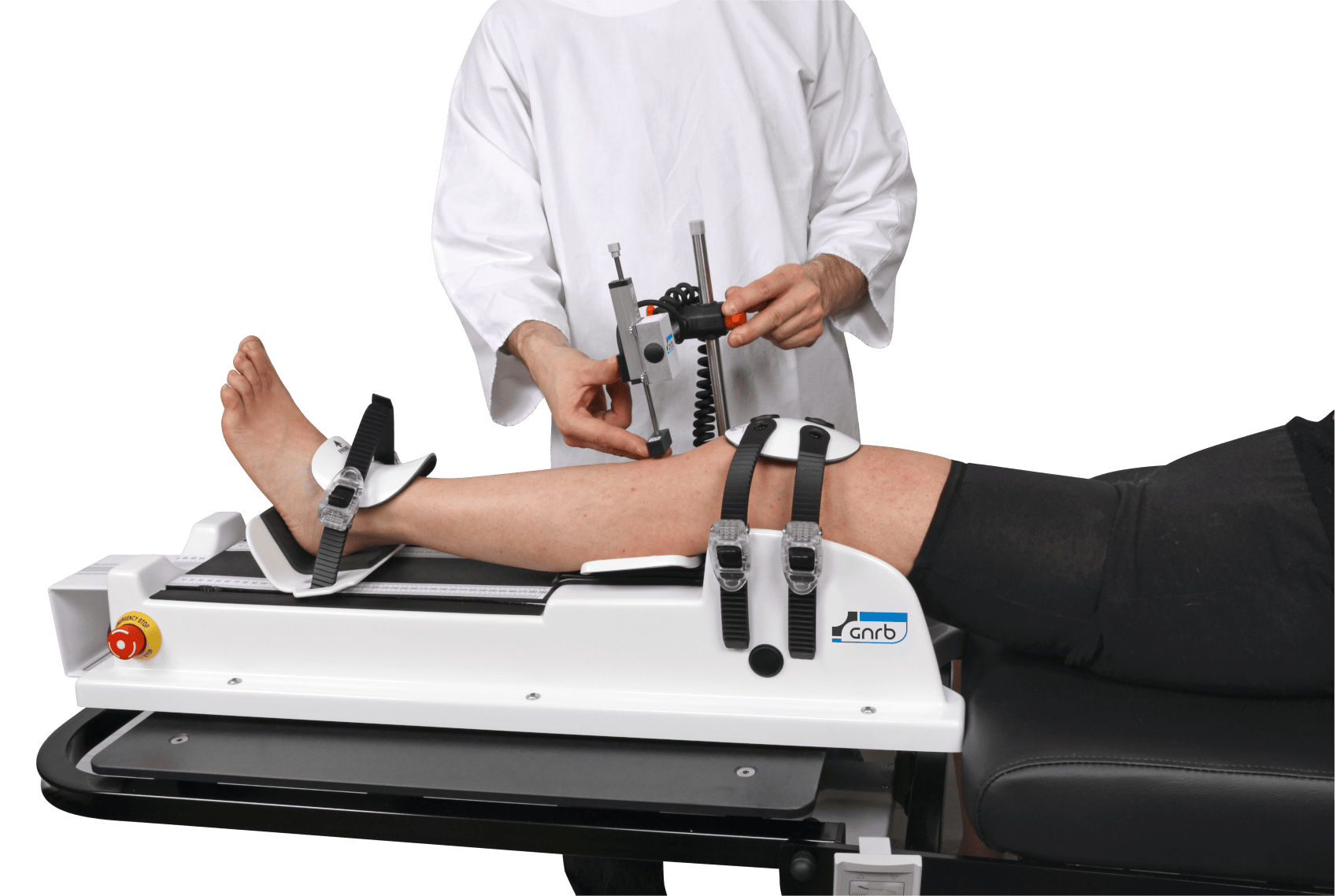
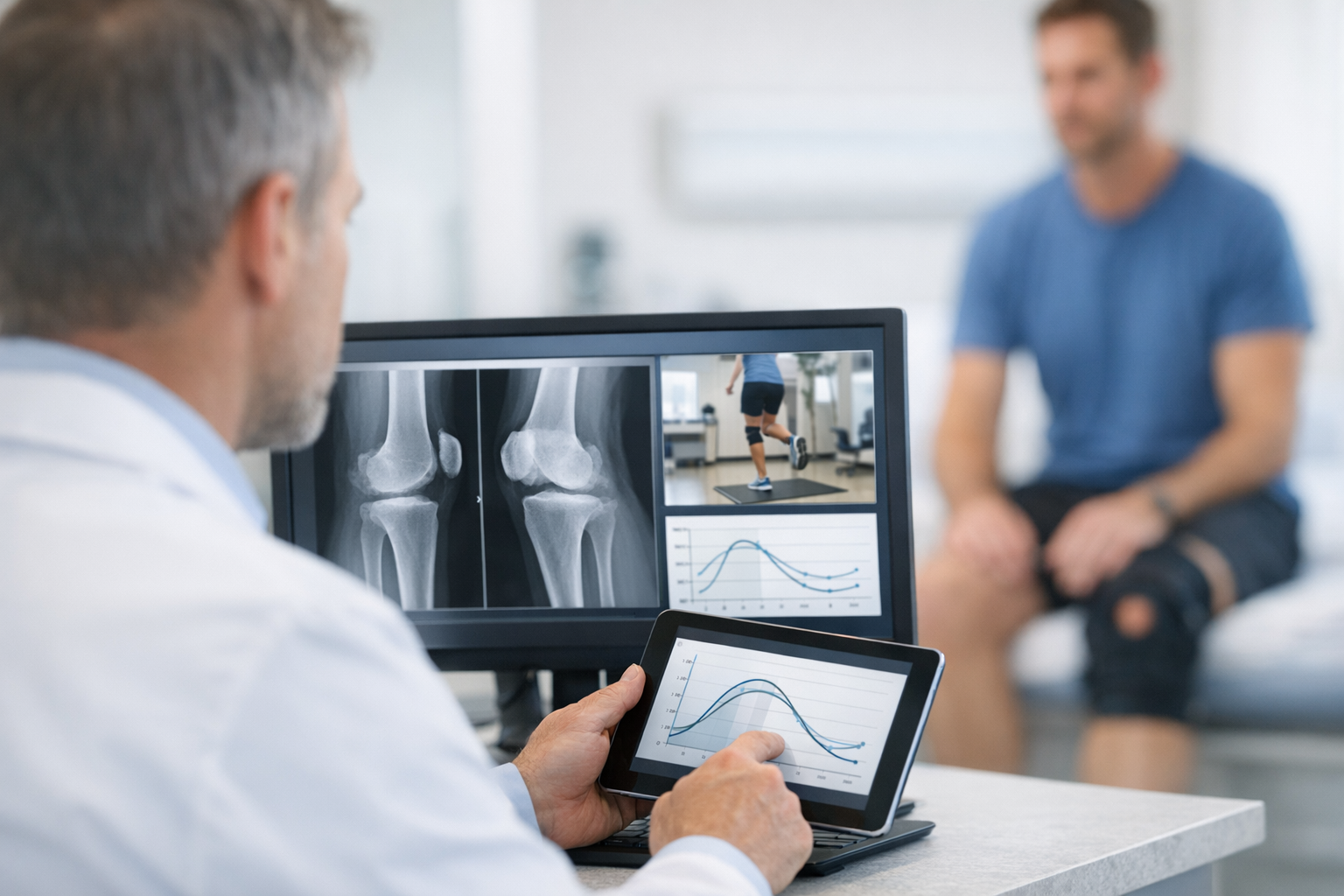
Because ACL graft stretch vs failure can sit on a continuum, objective testing may help clarify whether the knee demonstrates functionally meaningful side-to-side instability, particularly when symptoms and MRI are borderline. Instrumented assessment can complement clinical grading by quantifying translation across loads and supporting longitudinal tracking using devices such as the GNRB arthrometer for ACL assessment or the Dyneelax knee arthrometer.
When you interpret objective measures, remember that laxity alone does not fully describe functional stability. In some cases, stiffness or compliance characteristics may better represent graft behavior under load, which is why why stiffness and compliance can outperform laxity alone is a useful concept when the question is subtle elongation vs structural disruption.
How this helps the pivot shift conversation
- If the pivot shift is clearly positive and the objective anterior translation is only mildly increased, consider rotational contributors (PLC, lateral meniscus, LET deficiency, neuromuscular control) rather than assuming simple rupture.
- If objective translation is clearly increased and the endpoint is soft, the likelihood of structural compromise rises, but imaging is still needed to define associated injury and plan management.
Residual rotational laxity can persist even with an intact graft in select cases. For treatment context, Haque et al. (2026) reviews outcomes of isolated lateral extra-articular tenodesis for residual laxity following ACL reconstruction, which is relevant when instability is rotationally dominant and the intra-articular graft may appear intact.
Also keep graft construct considerations in mind. For example, augmentation strategies have been studied, including comparisons such as Antzoulas et al. (2026), though individual decisions remain patient-specific and surgeon-led.
5. Key takeaways and next steps
If you do only one thing when faced with ACL graft stretch vs failure, make it this: separate symptoms from measurable instability, then decide which additional information is needed to safely proceed.
- Do not over-rely on MRI alone: MRI is essential for associated injuries and planning, but functional instability may be clearer when paired with exam and objective measures.
- Trend matters: progressive side-to-side change is often more informative than a single visit result.
- Respect rotational instability: a pivot shift phenotype should trigger evaluation beyond the graft, including lateral meniscus and PLC contributors.
- Document explicitly: your note should state whether findings support elongation, rupture, or a non-graft explanation, and what would change management.
When to escalate (clinician-led, context dependent): recurrent giving way, inability to progress rehab due to instability, or objective instability consistent with ACL graft stretch vs failure plus imaging that supports graft compromise or significant associated injury. In those cases, the phrase revision ACL indications for graft failure should be translated into specific, documentable reasons: persistent symptomatic instability, unacceptable objective laxity, malpositioned tunnels, fixation issues, or meniscal and chondral injuries that demand stabilization to protect the knee.
Next steps can include: (1) repeat exam with standardized technique, (2) objective laxity measurement for baseline and follow-up, and (3) MRI to assess graft and concomitant pathology, then multidisciplinary discussion (sports physician, physiotherapist, surgeon) aligned to the athlete’s goals and sport demands. The goal is not to “label” quickly, but to reduce missed contributors and make ACL graft stretch vs failure a well-supported, auditable clinical conclusion.
6. Clinical references (PubMed)
1) 2026 – Haque et al. – Outcomes of Isolated Lateral Extra-articular Tenodesis for Residual Laxity Following ACL Reconstruction: A Systematic Review. – Orthop J Sports Med – DOI: 10.1177/23259671261416444 – PMID: 41783085 – PubMed
2) 2026 – Weiss et al. – Radiographic Measurement of Graft Bending Angle in Failed Anterior Cruciate Ligament Reconstructions: A Matched Control Analysis. – J Am Acad Orthop Surg Glob Res Rev – DOI: 10.5435/JAAOSGlobal-D-25-00470 – PMID: 41779927 – PubMed
3) 2026 – Capece et al. – Anterior Cruciate Ligament Reconstruction Failure: Etiology, Classification, and Revision Strategies-A Narrative Review. – J Funct Morphol Kinesiol – DOI: 10.3390/jfmk11010077 – PMID: 41718205 – PubMed
4) 2026 – Abu Mukh et al. – Sport-Specific Considerations in ACL Reconstruction: Diagnostic Evaluation and Graft Selection. – Diagnostics (Basel) – DOI: 10.3390/diagnostics16040584 – PMID: 41750733 – PubMed
5) 2026 – Antzoulas et al. – LARS-augmented hamstring ACL reconstruction shows better early but similar long-term outcomes compared with hamstring autograft alone: A systematic review and meta-analysis. – J Exp Orthop – DOI: 10.1002/jeo2.70654 – PMID: 41743308 – PubMed