Accurate pediatric ACL injury diagnosis is often harder than “small adult ACL” thinking suggests. Pain inhibition, apprehension, variable cooperation, and open physes can all distort the exam, while MRI can be challenged by partial injuries, developmental anatomy, and timing. When the clinical picture is uncertain, the priority is not just labeling a tear, but also identifying instability patterns, associated meniscal or chondral injury risk, and the most appropriate way to monitor change over time. This guide focuses on adolescent ACL rupture clinical exam pitfalls, rotational instability assessment, and how to build a safer, more objective follow-up strategy for children and adolescents.
1. Pediatric ACL injury diagnosis: Why kids are not “small adults”
In children, pediatric ACL injury diagnosis is frequently confounded by factors that reduce test validity and increase false reassurance. Even experienced clinicians can be misled when the exam is performed too early, on a guarded knee, or without appreciating pediatric injury patterns.
1.1 Key diagnostic “noise” that weakens the exam
- Guarding and pain inhibition: hamstring co-contraction can artificially limit anterior tibial translation.
- Physes and anatomy: developmental morphology can change the “feel” of endpoints and pivot behavior.
- Communication and anxiety: fear and poor tolerance can reduce sensitivity of manual tests.
- Timing: very acute hemarthrosis can limit ROM and reliability of laxity assessment.
To reduce avoidable misses, it can help to standardize documentation and reduce variability in the way instability is recorded, as outlined in an objective knee examination in orthopaedics.
1.2 Pediatric injury patterns that mimic or mask ACL rupture
A “tibial eminence avulsion” phenotype can present with laxity that overlaps with ACL insufficiency, and some children develop persistent symptoms that require structured reassessment rather than a one-time clearance. If you manage these injuries, see the discussion on knee laxity in children after anterior tibial eminence fracture and the value of longitudinal comparison.
For a broader overview of common pediatric pitfalls in pediatric ACL injury diagnosis, this resource on pediatric ACL diagnostic considerations and pitfalls complements the clinical points below.
1.3 Practice variation matters (and it is measurable)
Pathways differ across centers in terms of triage, documentation, and follow-up, which can influence timeliness and consistency of care. A UK multicentre audit highlighted real-world variation in practice and adherence to guidance in pediatric ACL care in Gompels et al. (2026), reinforcing the value of standardized assessment and tracking within local systems.
2. Clinical examination in children: Lachman, pivot shift, and rotational instability
The exam remains central to pediatric ACL injury diagnosis, but clinicians should actively manage test conditions (analgesia, reassurance, positioning, and time since injury) to improve interpretability. A practical approach is to document what you can trust today and what needs repeat testing when the knee is calmer.
Most clinicians still combine multiple tests rather than relying on any single maneuver. If you need a refresher set, this overview of the top ACL diagnostic tests can help align team language and documentation.
2.1 Lachman: useful, but easy to over-trust in guarded knees
Lachman remains a cornerstone, yet in young patients it may look “negative” when the child is resisting or when hamstrings are firing. Subtle increased translation with a seemingly “firm” endpoint can occur in partial injuries. For detailed nuance, including common misreads, review this Lachman test guide.
2.2 Pivot shift and rotational instability: interpretability vs feasibility
Rotational instability is often what families describe as “giving way,” but the exam maneuver that best reflects it can be difficult to perform in awake children. A careful pivot shift assessment in children may be limited by apprehension, pain, or muscle activation. If the clinical story suggests instability but the pivot shift is not assessable, document that limitation explicitly and consider reassessment later (or under anesthesia if clinically indicated) rather than concluding absence of instability.
When you do attempt the test, define what you mean by a “positive” result and how reproducible it is across examiners, because that context often determines how the information is used in decision-making.
3. MRI and growth plate considerations in suspected pediatric ACL tears
MRI is typically central for confirming a pediatric anterior cruciate ligament tear and for mapping associated injuries. It can also clarify differential diagnoses (osteochondral injury, bone bruising patterns, meniscal pathology) and inform surgical planning. However, MRI interpretation can be challenged by partial tears, evolving signal changes, and the reality that structure does not always predict function.
In equivocal scenarios, objective instability information may help clinicians interpret borderline findings, but it should be framed as complementary, not a replacement. A clinician-facing discussion of this “both-and” approach is provided in MRI vs arthrometer for improving ACL tear detection.
3.1 “Growth plate considerations ACL reconstruction” starts at diagnosis
The phrase growth plate considerations ACL reconstruction is not only about surgical technique selection. It starts earlier with: (1) precise characterization of instability patterns, (2) defining concomitant pathology that may worsen with delay, and (3) building a monitoring plan that can justify escalation or continued rehabilitation.
Delay can matter for associated injuries in adolescents. A retrospective cohort analysis linked age and time to surgery with concomitant meniscal injury patterns in Turati et al. (2026), supporting vigilant follow-up when instability is suspected or symptoms persist.
3.2 Decision aid for “equivocal exam” or “borderline MRI”
This is not a rigid pathway, but a practical decision aid when pediatric ACL injury diagnosis remains uncertain after initial work-up:
- Re-examine when pain and effusion are better controlled, documenting ROM, endpoint quality, and tolerance.
- Clarify instability history (giving-way episodes, direction of collapse, pivoting triggers, confidence with cutting).
- Actively screen for associated injury (locking, joint line tenderness, mechanical symptoms) and use MRI where indicated for meniscus/cartilage/bone assessment.
- Plan objective follow-up rather than “watch and wait” without measurable endpoints, especially if sport demands are high.
- Escalate appropriately if instability episodes continue, function deteriorates, or exam findings evolve.
Also consider access factors. Disparities work in pediatric sports medicine, including how we define and study neighborhood-level metrics, is discussed in Maxwell et al. (2026), and is relevant when delays or missed follow-up are recurring barriers.
4. Pediatric ACL injury diagnosis and follow-up: Quantifying laxity over time
Even after a careful work-up, many clinicians still face “gray zone” cases where symptoms, exam, and imaging do not align. In these cases, pediatric ACL injury diagnosis often benefits from tracking change rather than forcing certainty at one visit. This is particularly useful when you suspect partial injury, when the child cannot relax, or when rehabilitation is underway and you want to confirm that stability and function are moving in the right direction.
Two phrases are worth operationalizing in your notes: pediatric knee laxity measurement and objective ACL follow-up monitoring. Together, they shift follow-up from impression-based to trend-based.
4.1 What to measure, and how to report it
When laxity is measured, clinicians commonly describe an anterior tibial translation side-to-side difference and interpret it alongside symptoms, strength, and movement quality. Regardless of device or method, the same interpretation principles apply:
- Side-to-side comparison is often more informative than an absolute value in a growing child.
- Consistency (same set-up, same knee position, same force targets) matters for longitudinal interpretation.
- Trend matters: stable, improving, or worsening measurements should change your clinical confidence.
For a plain-language overview of methods and terminology, see this explanation of knee laxity testing and how it supports structured documentation.
4.2 Where instrumented arthrometers fit (complementary to MRI and exam)
Instrumented testing can add objective, repeatable data to the clinical picture, particularly when manual exams are limited by guarding or when you need reproducible follow-up points; this is one reason clinicians discuss the arthrometer role in ACL diagnostics as a complement to clinical tests and MRI rather than a substitute.
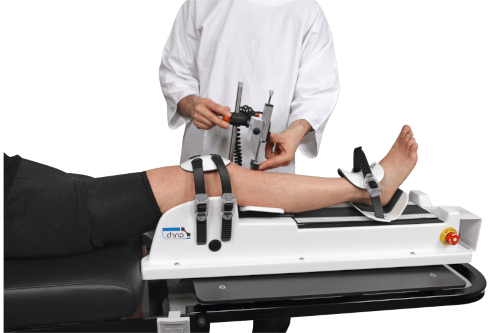
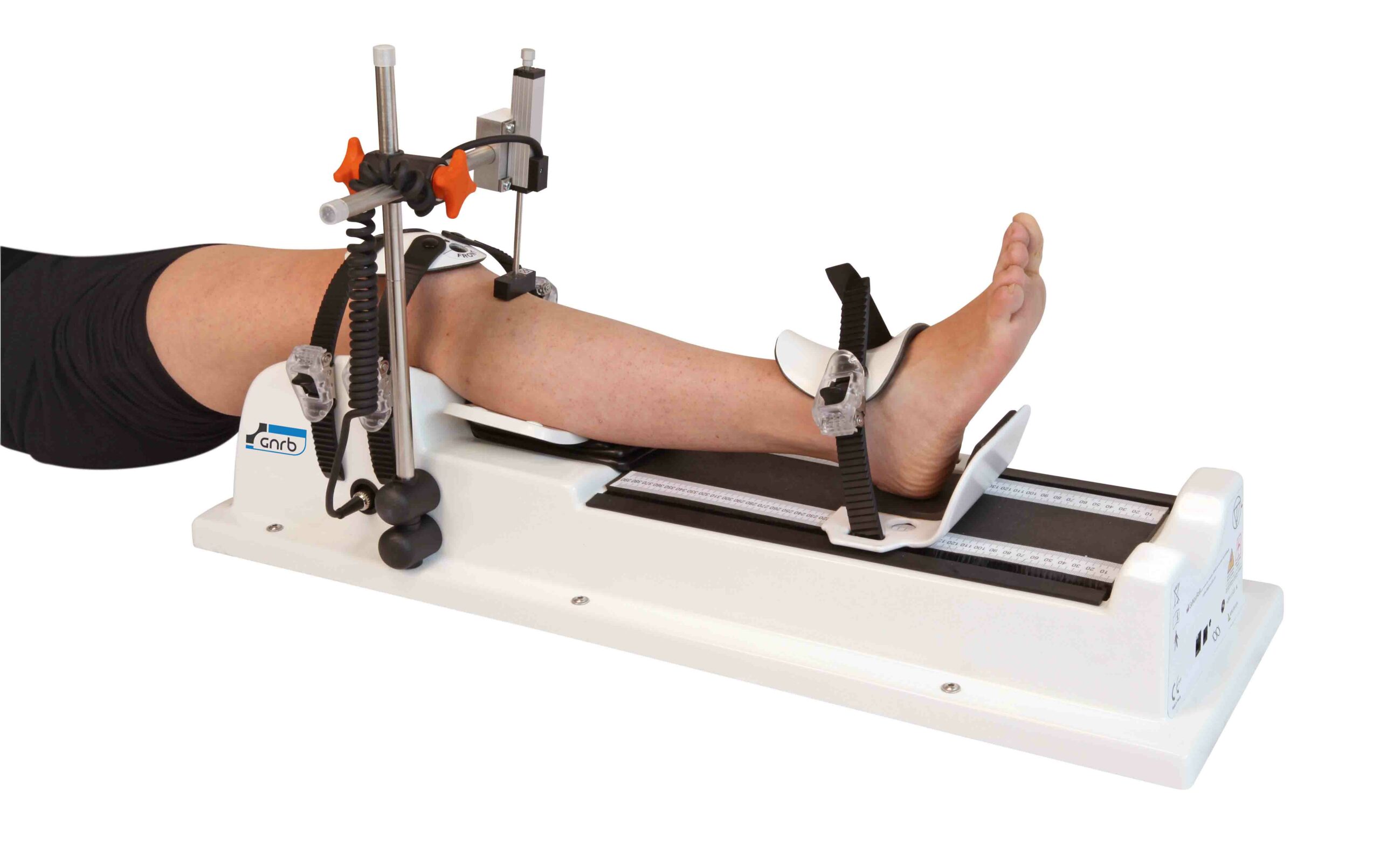
In clinics that use robotic or instrumented tools, examples include the GNRB arthrometer for ACL assessment and the Dyneelax knee arthrometer, which may support serial comparison when the goal is objective monitoring rather than a one-time snapshot.
Reliability is not automatic. If you are implementing instrumented measures in follow-up protocols, ensure staff training and consistency, and be aware of measurement variability and operator effects discussed in the GNRB learning curve for ACL measurement.
4.3 Linking laxity to tissue and outcomes (research direction)
Objective laxity outcomes are increasingly being related to imaging biomarkers and graft maturation concepts. For example, an early post-operative research link between quantitative MRI parameters and normalized laxity has been explored in quantitative MRI UTE-T2 and BMI-normalized knee laxity, illustrating how “structure plus function” may refine follow-up interpretation over time. In day-to-day pediatrics, the practical takeaway is to keep MRI for associated injury assessment and planning, while using objective measures to document functional stability changes.
5. Outcomes, return to sport, and what to track after pediatric ACL injury
Families often ask for a single clearance test, but pediatric ACL injury diagnosis and subsequent management are safer when return decisions reflect multiple domains: symptoms, objective stability, strength, neuromuscular control, psychological readiness, and sport demands. The keyword phrase return to sport after pediatric ACL should be treated as a staged process, not a date.
5.1 PROMs and child-specific reporting
Child-appropriate patient-reported measures help separate pain, symptoms, function, and confidence, especially when objective findings and athlete perception diverge. A pediatric-specific PROM underwent validation and item reduction work in Hansen et al. (2026), supporting the principle that children and adolescents should be assessed with tools designed for their context, not only adult instruments.
5.2 Surgical techniques and growth-related safety considerations
When reconstruction is indicated in skeletally immature athletes, technique selection aims to balance stability restoration with physeal safety. Mid- to long-term outcomes for an all-epiphyseal, all-inside approach with high return-to-sport and minimal growth-related complications were reported in Ntagiopoulos et al. (2026). This does not remove the need for individualized planning, but it supports ongoing refinement of pediatric options.
5.3 Key takeaways and next steps
- Do not over-interpret a single “negative” manual test in a guarded child; document limitations and reassess.
- Use MRI to evaluate associated injury and support planning, while acknowledging that functional instability may not be fully captured on imaging.
- Build follow-up around objective ACL follow-up monitoring and consistent documentation, especially when initial certainty is low.
- Track outcomes with child-appropriate PROMs and staged, criterion-based return-to-sport decisions.
If you are handing over care (ED to clinic, clinic to physiotherapy, or physiotherapy back to surgeon), ensure your notes clearly state the current confidence in pediatric ACL injury diagnosis, what remains uncertain, and what measurable criteria will trigger escalation or de-escalation.
Clinical references (PubMed)
1) 2026 – Gompels et al. – The Paediatric ACL National Audit (PANA) study: a multicentre review of UK practice and adherence to BOAST guidelines. – Knee – DOI: 10.1016/j.knee.2026.104390 – PMID: 41747609 – PubMed
2) 2026 – Hansen et al. – The KIDS-KNEES-ACL is a valid PROM for children and adolescents with an ACL injury; item reduction using Rasch analysis and confirmatory factor analysis. – Knee Surgery, Sports Traumatology, Arthroscopy – DOI: 10.1002/ksa.70343 – PMID: 41711553 – PubMed
3) 2026 – Turati et al. – Age and Time to Surgery Are Associated with Concomitant Meniscal Injuries in Adolescent ACL Tears: A Retrospective Cohort Study. – Healthcare (Basel) – DOI: 10.3390/healthcare14040491 – PMID: 41754004 – PubMed
4) 2026 – Ntagiopoulos et al. – All-epiphyseal, all-inside ACL reconstruction yields high return-to-sport and minimal growth-related complications at mid- to long-term follow-up in skeletally immature patients. – Journal of Experimental Orthopaedics – DOI: 10.1002/jeo2.70671 – PMID: 41768533 – PubMed
5) 2026 – Maxwell et al. – Which Neighborhood-level Metric Is Most Appropriate for Pediatric Sports Medicine Disparities Research? – Clinical Orthopaedics and Related Research – DOI: 10.1097/CORR.0000000000003857 – PMID: 41758679 – PubMed