Return-to-sport decisions after ACL injury or reconstruction are rarely limited by one variable. Even when an athlete “passes” strength and hop testing, persistent functional instability can remain clinically relevant, particularly for cutting and pivoting sports. Modern ACL return to sport criteria increasingly aim to triangulate performance capacity (strength, hops, movement quality) with symptoms, psychology, and objective measures of knee stability. This guide focuses on how objective knee stability testing can complement strength testing, especially when the story, exam, and imaging are not fully aligned. The goal is not to replace clinician judgement, but to reduce uncertainty, document progression, and support shared decision-making around risk.
ACL return to sport criteria: why strength-only clearance can fail
Most clinicians have seen the “strong but unstable” athlete: good gym numbers and symmetry on paper, yet ongoing giving-way, loss of trust during deceleration, or a clearly abnormal pivot phenomenon. Here’s the catch: strength tests largely quantify capacity, not the ligament’s restraining function under rapid anterior and rotatory loads.
When discussing ACL return to sport criteria, it can help to separate three questions:
- Can the athlete generate force and absorb load? (strength and power)
- Does the knee remain stable under translation and rotation demands? (stability and laxity)
- Will the athlete execute sport tasks safely in real environments? (movement strategy, exposure, confidence)
This matters because many proposed ACL re-injury risk predictors are multifactorial: they involve neuromuscular control, graft and tissue factors, sport exposure, psychological readiness, and residual instability. For background on why reinjury and failure remain clinically important even with good rehabilitation, see ACL reinjury and surgery failure relapse.
Strength and functional performance: interpreting LSI, hop tests, and quality
Strength criteria are foundational, but interpretation needs nuance. A quadriceps strength limb symmetry index can be informative, yet symmetry alone may overestimate readiness if both limbs are deconditioned, or if the athlete compensates with hip strategy. Similarly, the hop test return to sport battery is useful, but can be “passed” with stiff-knee landings, trunk compensations, or avoidance of knee flexion moments.
Practical interpretation points
- Match the test to the sport: linear hop symmetry is less specific for high-demand pivoting loads.
- Do not ignore movement quality: consider valgus collapse, trunk lean, braking strategy, and asymmetrical knee flexion.
- Account for sex-specific recovery patterns: quadriceps recovery can be slower in some groups, influencing timing and exposure planning. In a systematic review and meta-analysis, Sharma et al. (2026) reported slower quadriceps strength recovery in female patients after quadriceps tendon autograft compared with male patients, alongside equivalent graft failure but lower activity scores.
Muscle properties also matter for stability behavior. If you want a deeper mechanistic angle on how soft tissue stiffness can influence translation control, see hamstring stiffness and anterior tibial translation control.
Finally, strength testing should be interpreted alongside symptoms and context: effusion, pain, ROM deficits, and apprehension can all reduce the validity of a “pass.” Where fear avoidance or hesitation is prominent, readiness discussions may need to consider the interaction between objective findings and psychological factors such as laxity and kinesiophobia.
Objective knee stability testing: translating laxity into RTS decisions
Objective knee stability testing aims to quantify translation response in a way that complements the manual exam. In practice, it can be particularly helpful when clinical exam is limited by guarding, when a patient reports instability despite strong performance tests, or when the side-to-side picture is unclear.
Two concepts tend to show up in clinical workflows:
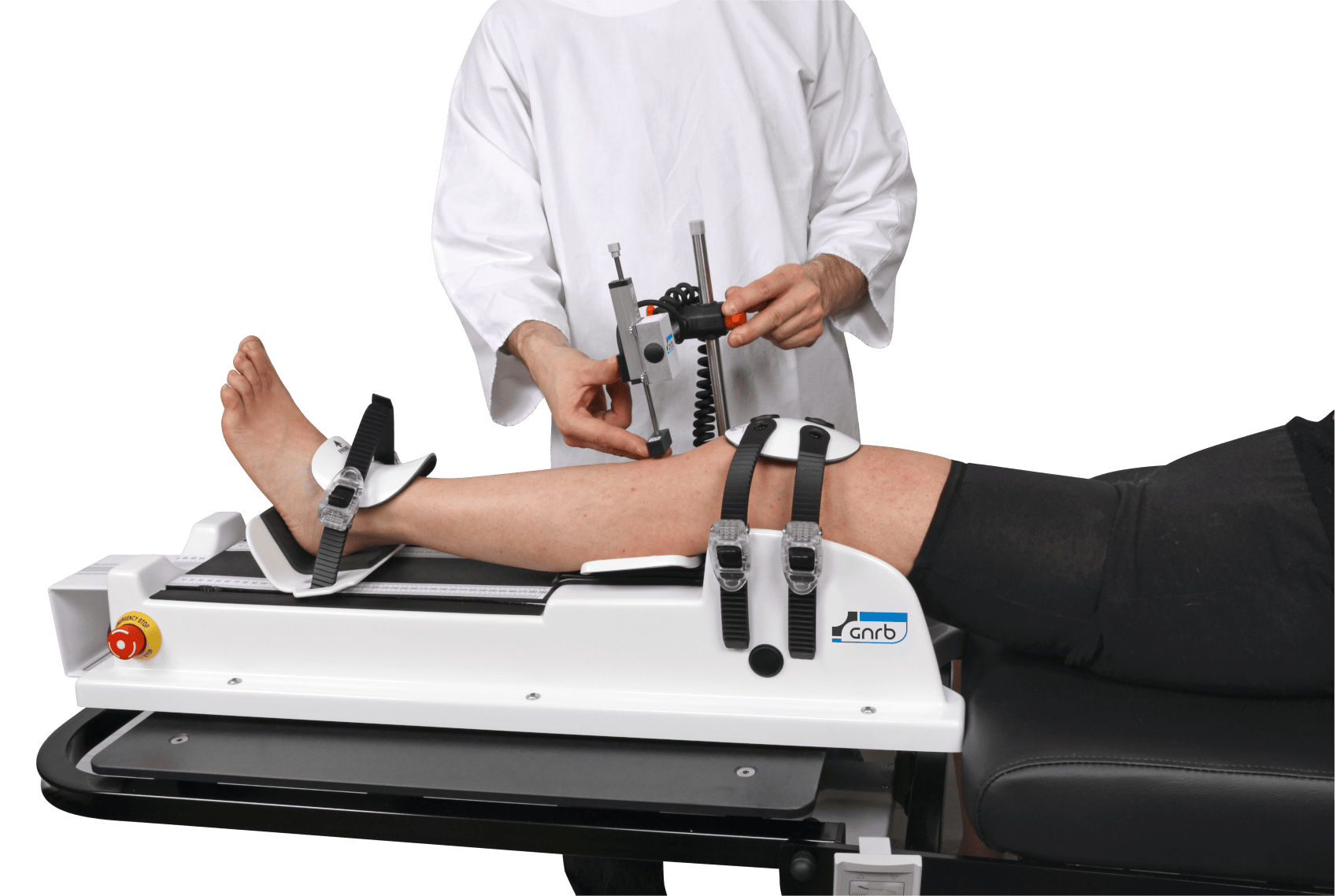
- instrumented anterior tibial translation: quantifying anterior displacement under standardized loads.
- side-to-side difference ACL laxity: comparing the involved to the uninvolved limb to contextualize the number.
These measurements can be documented over time, which is relevant to how ACL return to sport criteria evolve through late-stage rehab and during exposure ramp-up. For an overview of how objective data are typically captured and interpreted in clinical settings, see objective laxity measures to complement strength criteria.
Why stiffness metrics are increasingly discussed
Translation at one load does not fully describe how the knee behaves across the force range. Some clinicians also consider compliance or stiffness-based outputs because they may better represent the functional restraint response of the graft-ligament complex. A useful discussion is available on ACL compliance and stiffness metrics, which can be considered alongside (not instead of) symptoms, exam, and imaging.
How to use objective stability in an RTS conversation
Objective stability is not a single “green light.” Rather, it can:
- Clarify whether “good strength” is paired with stable mechanics under controlled translation loads.
- Support clinician-led decisions about sport-specific progression (for example, delaying cutting volume if stability remains borderline).
- Provide a repeatable data point to align the team (surgeon, physio, S&C, athlete) when ACL return to sport criteria are debated.
Objective testing should be framed as complementary to MRI and clinical examination. MRI remains important to evaluate meniscus, cartilage, bone bruising patterns, and for surgical planning when reconstruction is being considered. Objective stability data can add functional context, especially in borderline or suspected partial tears, but it does not replace imaging.
Longitudinal interpretation can also be paired with graft maturation concepts. For example, graft maturation imaging and measured laxity highlights how imaging biomarkers and measured laxity can be examined together within the first year after ACL reconstruction.
Rotational instability: pivot shift, landing mechanics, and dynamic laxity
Cutting and pivoting injuries are not just “anterior translation problems.” pivot shift rotational instability reflects a combined translational and rotational phenomenon and is often closer to the athlete’s symptom of giving-way than a pure sagittal plane measure. A clinician’s pivot shift grading is valuable, but can vary with examiner technique, patient relaxation, and concomitant injury patterns.
That is where dynamic knee laxity assessment can add context: it seeks to quantify how the knee behaves when the system is stressed in a way that better resembles sport demands than static strength tests alone. For a deeper look at approaches that go beyond static measures, see dynamic stability assessment.
Common pitfalls when rotational findings do not match “passing” strength
- Residual lateral or anterolateral laxity contributing to a pivot phenomenon despite good quadriceps symmetry.
- Meniscal deficiency (especially posterior horn involvement) altering stability, confidence, and load tolerance.
- Movement strategy that masks symptoms in tests but fails under fatigue, reactive decision-making, or unplanned cutting.
Surgical technique can also influence rotational stability strategies in selected patients. For example, Carrozzo et al. (2026) reported that lateral extra-articular tenodesis in high-risk patients after primary ACL repair was associated with protection from re-rupture risk and improved patient-reported outcomes in their cohort. The key RTS takeaway is not that one procedure “solves” risk, but that patient selection, surgical construct, and objective stability can influence how conservative or aggressive late-stage progression should be.
Tech integration: instrumented testing across diagnosis to prevention
When clinicians include robotic arthrometry within ACL return to sport criteria, the intent is typically to complement manual exam and MRI with repeatable quantification.
1) Diagnostic support: In equivocal or suspected partial ACL cases, instrumented testing may help quantify functional instability (for example, translation response and side-to-side differences) that imaging may not fully capture. MRI remains complementary and is typically needed to assess associated injuries and support operative planning.
2) Surgical planning: Pre-operative or pre-rehab baseline translation and rotational findings can help describe the functional instability phenotype and support discussions about graft choice, augmentation, or addressing concomitant pathology, without over-interpreting any single metric.
3) Post-operative monitoring: Serial measures can track changes in translation response during rehabilitation and graft maturation, providing context when performance tests improve but symptoms persist, or when an athlete regresses after load increases.
4) Prevention and screening: In at-risk athletes or those with prior injury, objective baselines may support monitoring over time and inform targeted neuromuscular programs, while avoiding claims that any tool can “predict” injury in isolation.
Clinics that choose device-based workflows often use tools such as the GNRB arthrometer for instrumented anterior tibial translation or the Dyneelax knee arthrometer for objective laxity tracking. Whatever the system, reliability depends on protocol, positioning, patient relaxation, and operator training. Practical implementation considerations are discussed in the GNRB learning curve for ACL measurement, and broader context comparing clinical options is summarized in a comparative analysis of KT-1000 and newer arthrometers.
A clinic-ready decision aid using ACL return to sport criteria
A useful way to think about RTS clearance is as a tiered decision: capacity, control, and confidence under sport exposure. Below is a practical structure that keeps ACL return to sport criteria comprehensive without becoming unworkable.
Stepwise RTS decision aid (practical, clinician-led)
-
Confirm prerequisites: quiet knee (minimal effusion), full extension, near-normal flexion, and tolerable symptom response to progressive field work.
-
Capacity: strength testing (including quadriceps symmetry and rate of force development where available) plus a hop battery interpreted with movement quality, not distance alone.
-
Control: screen for valgus collapse, trunk control, deceleration mechanics, fatigue effects, and sport-specific task execution (planned and unplanned where safe).
-
Stability phenotype: integrate manual exam (Lachman, anterior drawer, pivot shift) with objective translation measures if available, particularly when the athlete reports instability or the exam is borderline.
-
Risk conversation: review patient-specific modifiers (age, sport, prior injury, contralateral risk, concomitant meniscus or cartilage injury, adherence). Use objective data to document uncertainty rather than to force a binary decision.
Where the surgical literature informs RTS discussions (without overpromising)
-
Repair vs reconstruction decisions can influence timelines and expectations, but RTS varies widely across studies and protocols. A systematic review and meta-analysis by Annibaldi et al. (2025) evaluated return to sport and outcomes after arthroscopic ACL repair versus reconstruction, supporting nuanced, individualized discussions rather than one-size-fits-all timelines.
-
Construct choices and augmentation strategies may change early recovery profiles in some cohorts. Antzoulas et al. (2026) reported better early but similar long-term outcomes for LARS-augmented hamstring ACL reconstruction compared with hamstring autograft alone, which can be relevant when counseling about early function versus long-term equivalence.
-
Graft sizing strategies may matter for certain patients. Mancino et al. (2026) reported that using additional strands to increase graft diameter provided optimal outcomes without compromising healing at 12 months follow-up in their study context.
To keep the RTS exam consistent and defensible across clinicians, consider adopting an objective knee examination framework that standardizes what is measured, when it is measured, and how results are communicated to the athlete and care team.
Key takeaways and next steps
- Strength symmetry is necessary but not sufficient for many pivoting athletes.
- Objective measures can help document stability progression and refine how you interpret performance testing within ACL return to sport criteria.
- Rotational findings, including pivot shift behavior and dynamic control, should be explicitly addressed when planning cutting and contact exposure.
- When uncertainty remains, the safest next step is often to adjust exposure and retest rather than forcing a binary “cleared” decision.
Clinical references (PubMed)
1) 2026 – Sharma et al. – Anterior Cruciate Ligament Reconstruction With a Quadriceps Tendon Autograft in Female Patients Shows Equivalent Graft Failure But Lower Activity Scores and Slower Quadriceps Strength Recovery Compared With Male Patients: A Systematic Review and Meta-analysis. – Am J Sports Med – DOI: 10.1177/03635465251376649 – PMID: 41521740 – PubMed
2) 2025 – Annibaldi et al. – Return to sport and clinical outcomes after arthroscopic anterior cruciate ligament repair versus reconstruction: A systematic review and meta-analysis. – Knee Surg Sports Traumatol Arthrosc – DOI: 10.1002/ksa.70233 – PMID: 41451660 – PubMed
3) 2026 – Antzoulas et al. – LARS-augmented hamstring ACL reconstruction shows better early but similar long-term outcomes compared with hamstring autograft alone: A systematic review and meta-analysis. – J Exp Orthop – DOI: 10.1002/jeo2.70654 – PMID: 41743308 – PubMed
4) 2026 – Mancino et al. – The use of additional strands to increase graft diameter in primary ACL reconstruction provides optimal outcomes and does not compromise healing at 12-months follow-up. – Eur J Orthop Surg Traumatol – DOI: 10.1007/s00590-025-04653-2 – PMID: 41528525 – PubMed
5) 2026 – Carrozzo et al. – Lateral extra-articular tenodesis protects high-risk patients from the risk of re-rupture and improves patient-reported outcomes after primary anterior cruciate ligament repair: A retrospective cohort study with ≥2-year follow up. – Knee – DOI: 10.1016/j.knee.2025.11.014 – PMID: 41344957 – PubMed